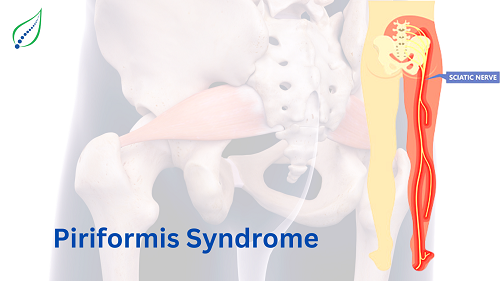
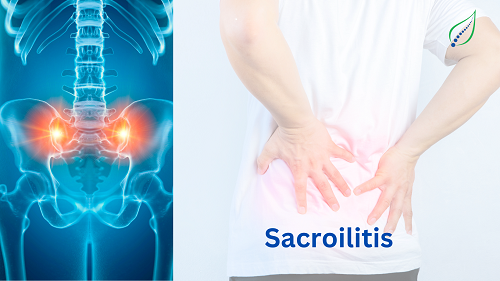
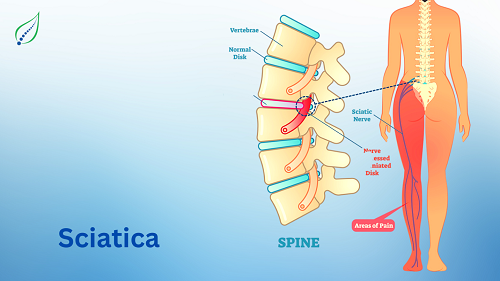
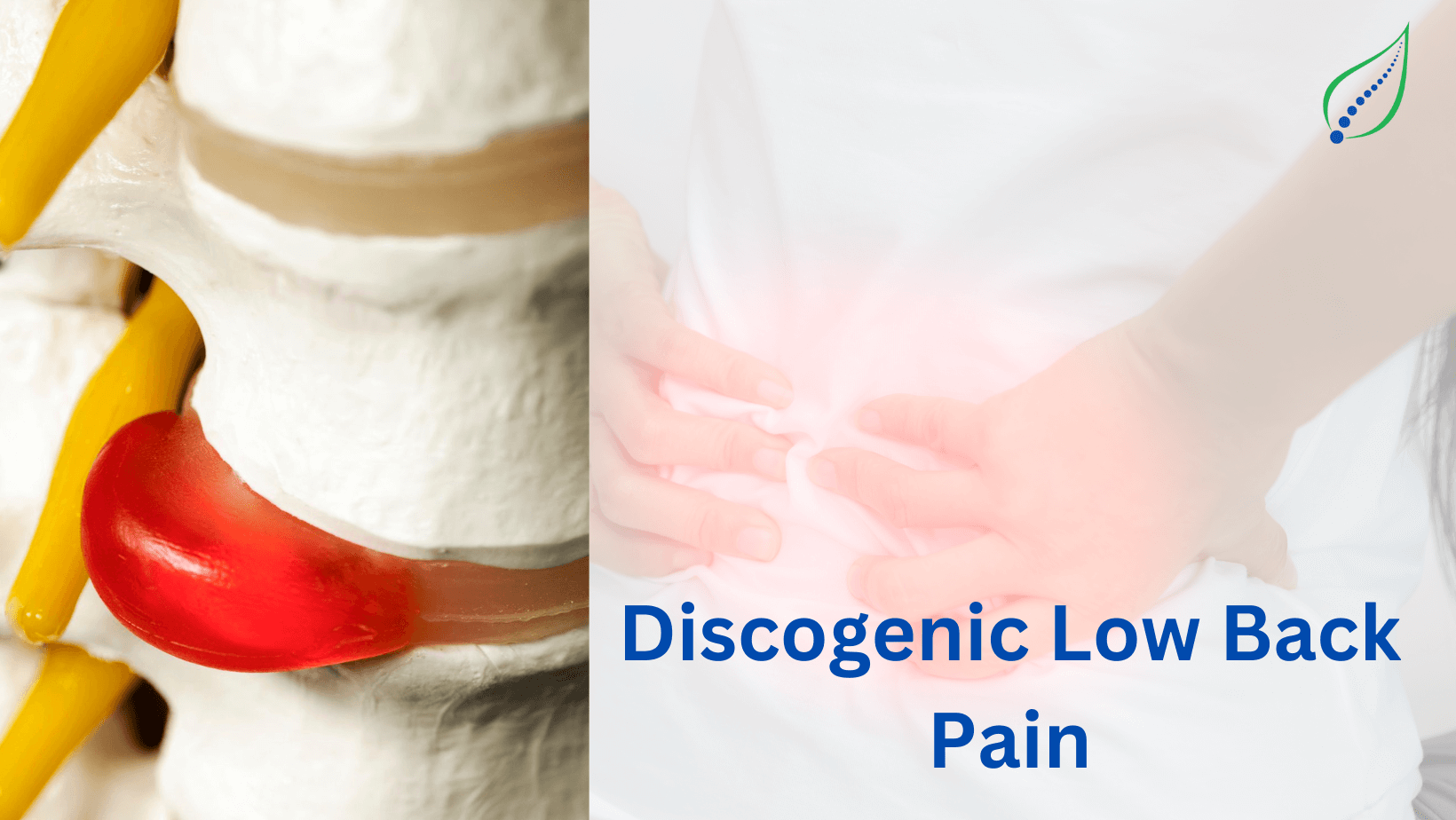
Low Back Pain

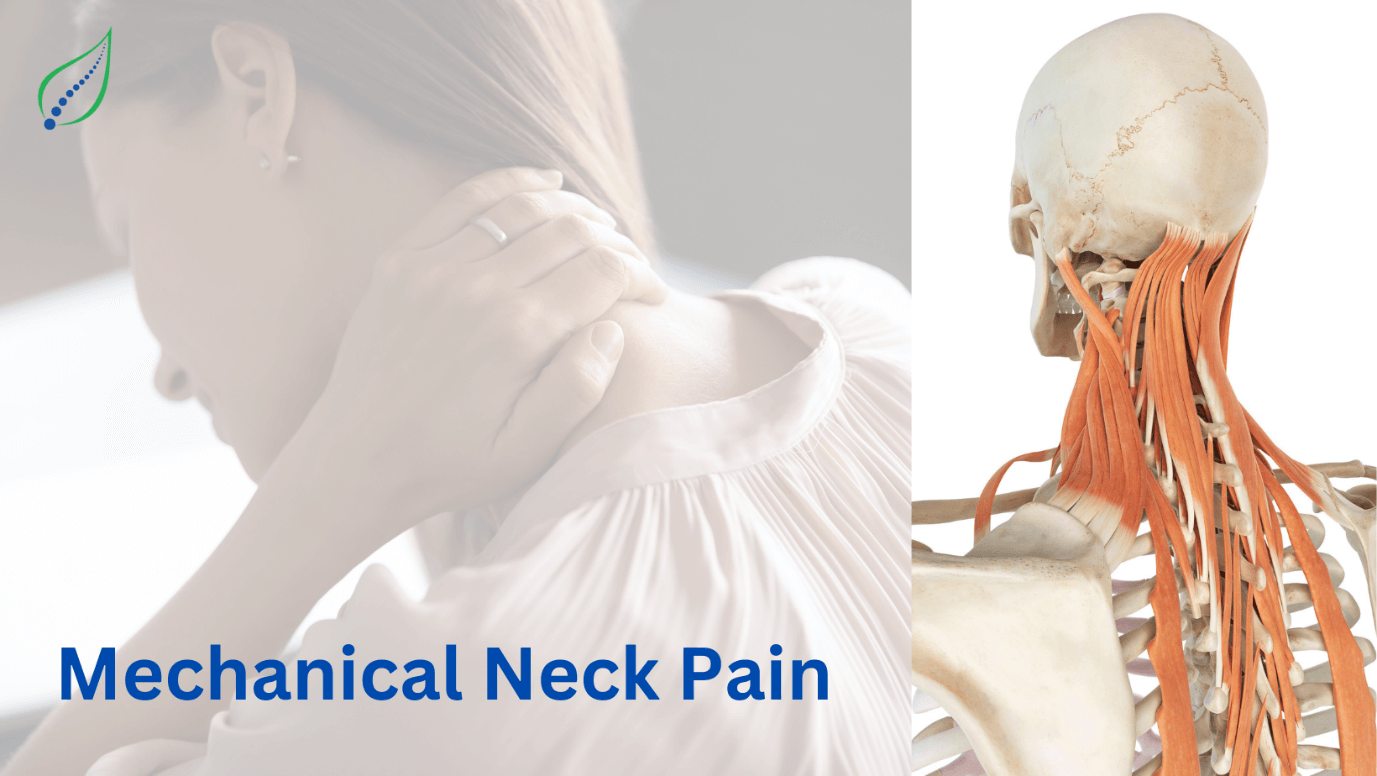
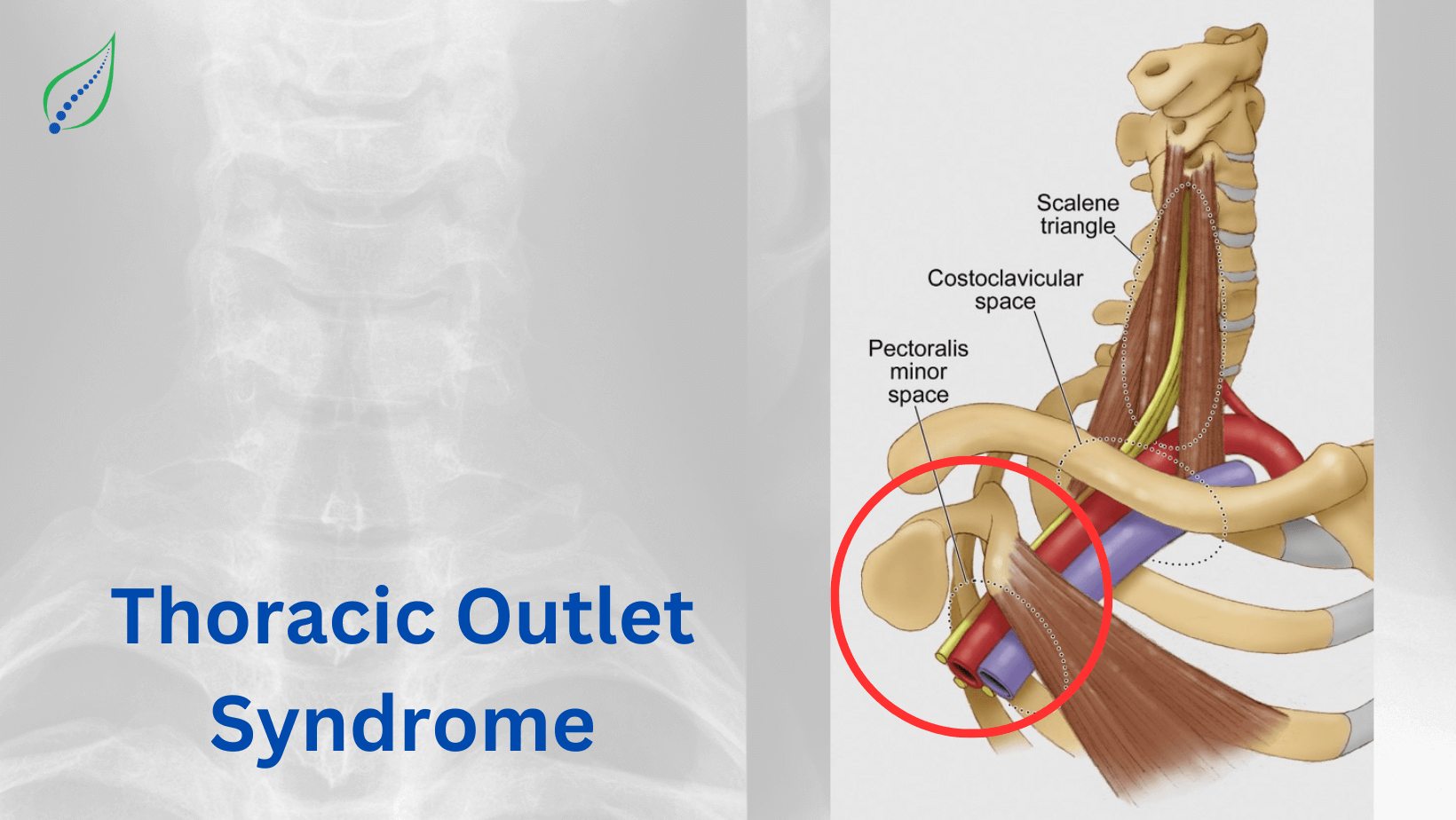
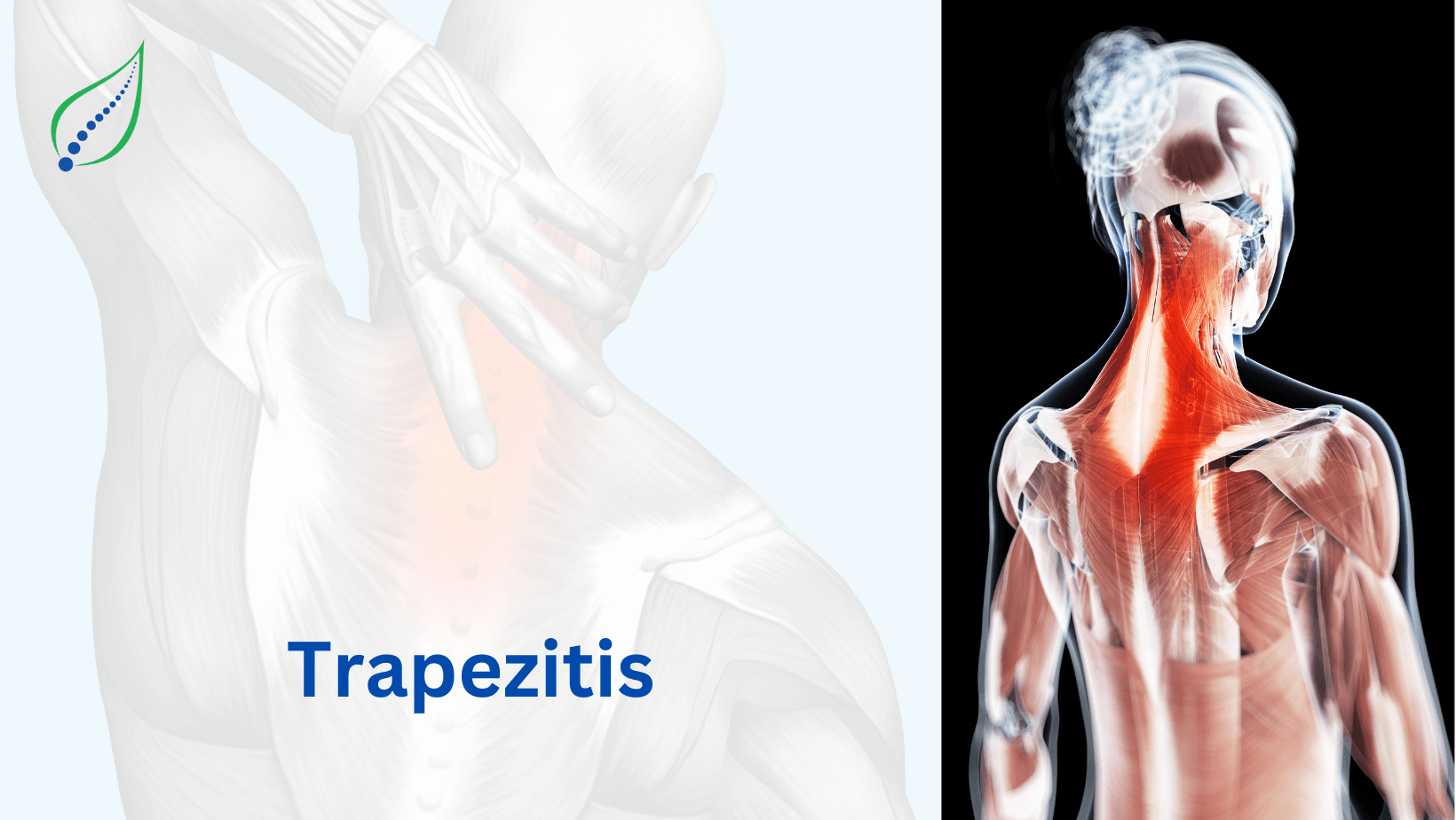
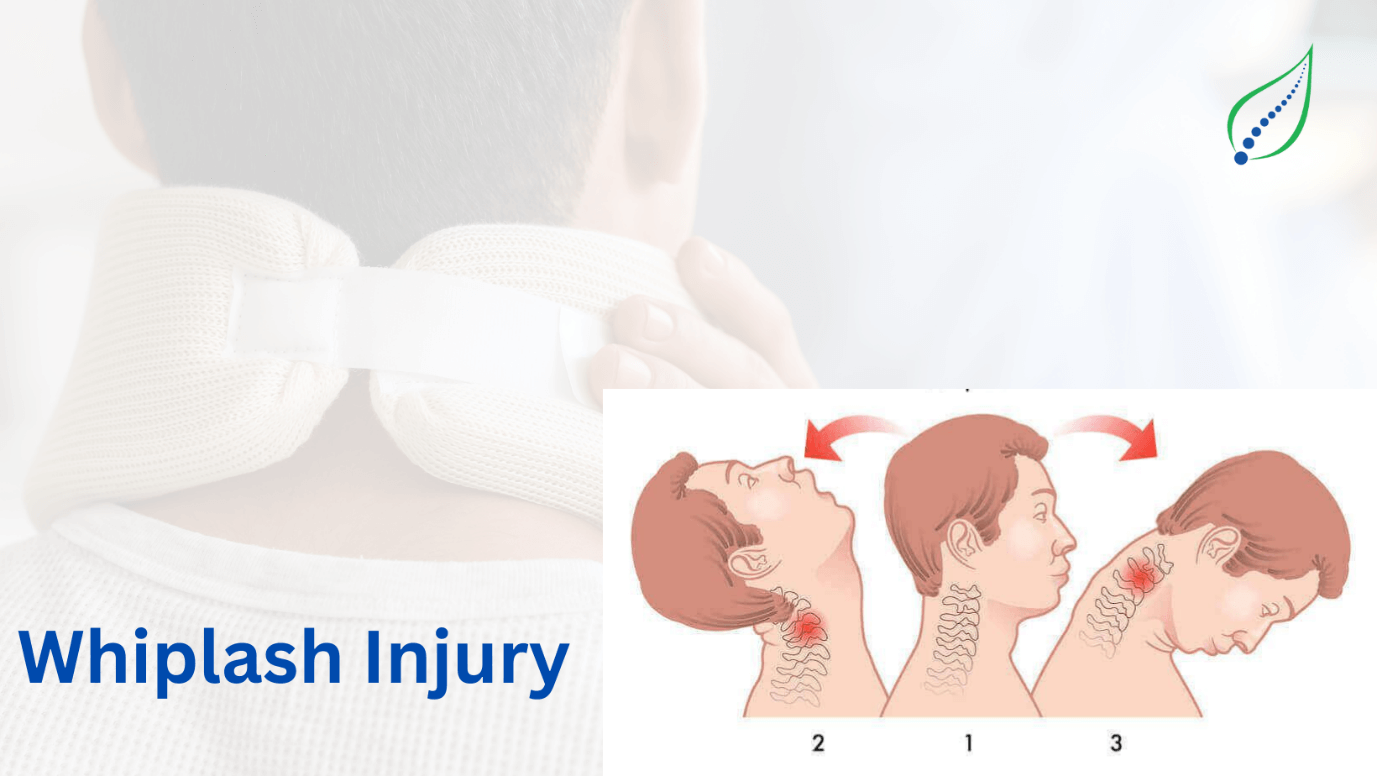
Neck Pain
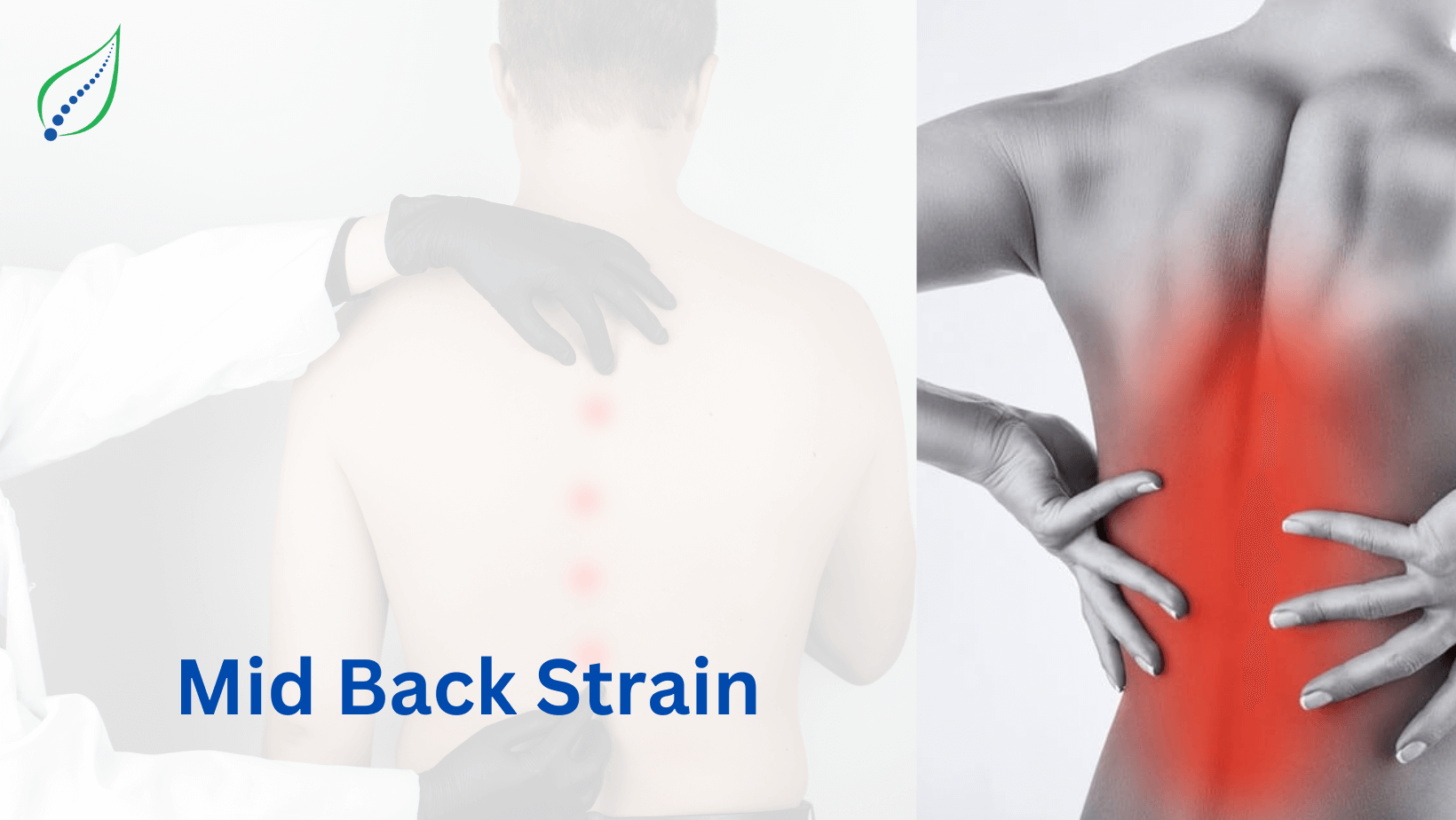
Mid Back Pain

Shoulder Pain
Knee Pain
Hip Pain
Elbow Pain
Hand & Wrist Pain

Ankle and Foot Pain

Headache
Leg Pain
Arthritis

Neuropathy

Other
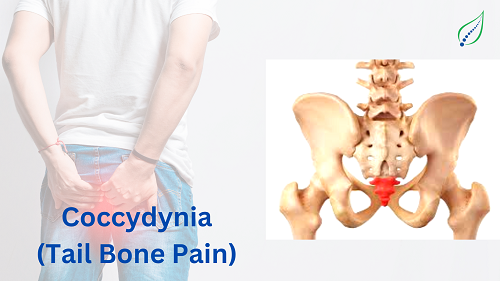
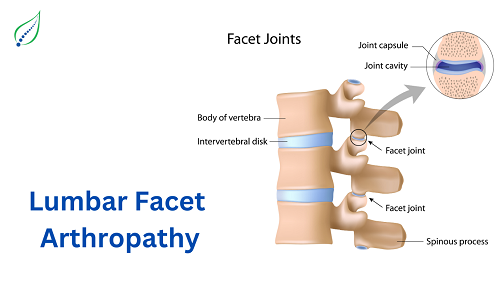
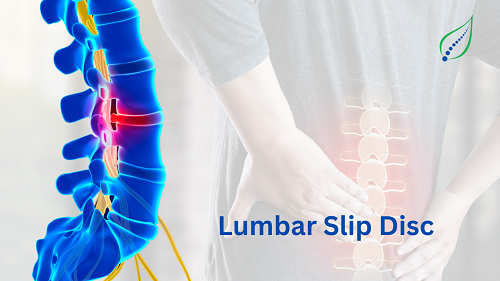
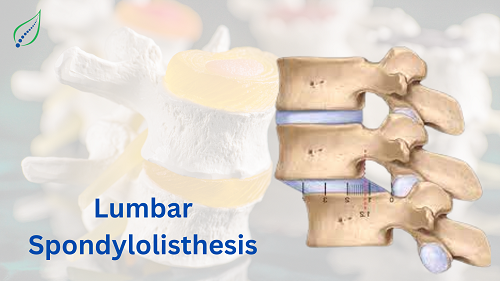
Low Back Pain
Neck Pain
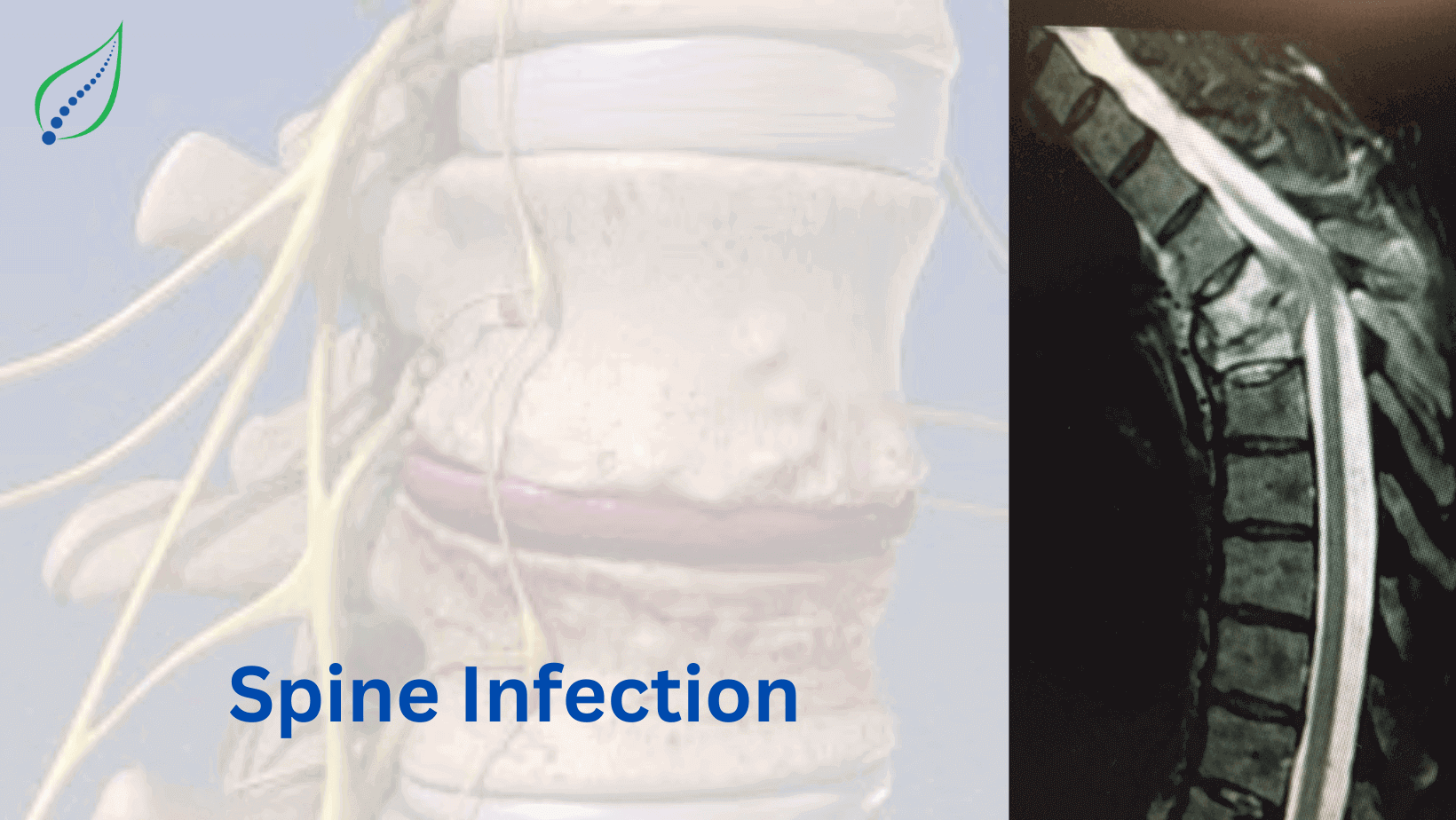
Cervical Spinal Canal Stenosis
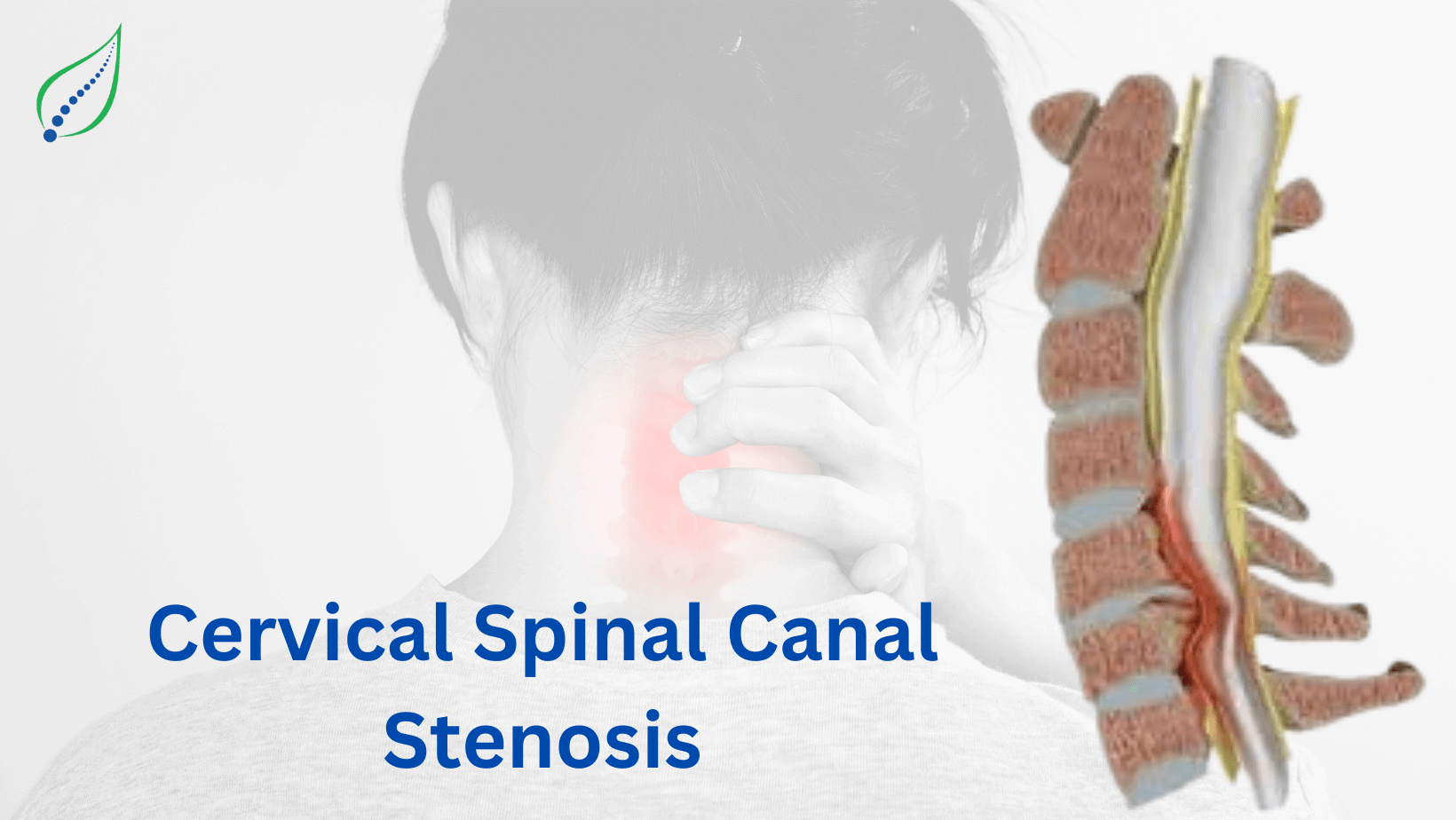
Cervical Spinal Canal Stenosis
Cervical spinal canal stenosis is the narrowing of the cervical spinal canal which results in the compression of spinal cord and nerve roots leading to degenerative changes in the cervical spine. It may be the result of traumatic and inflammatory conditions caused by herniated disc.
Mid Back Pain
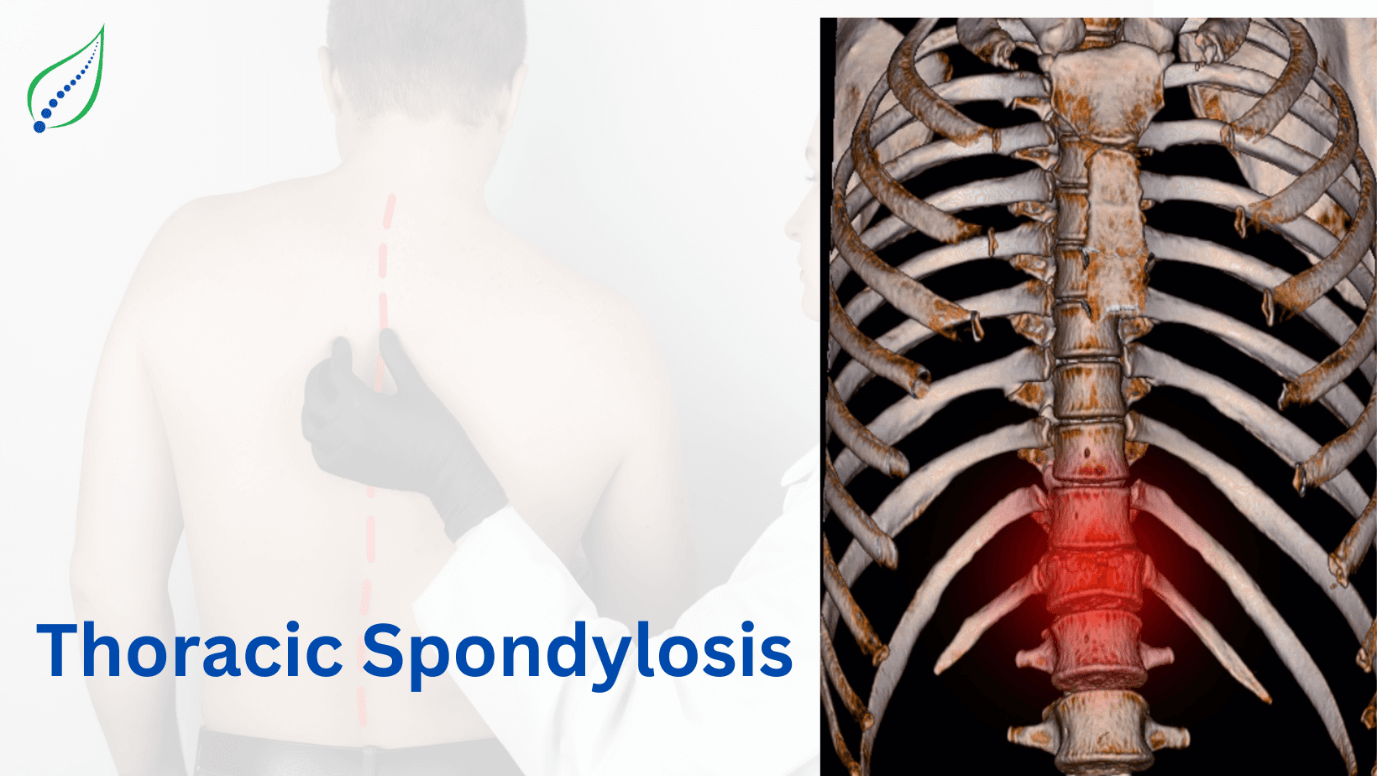
Scheuermann Disease
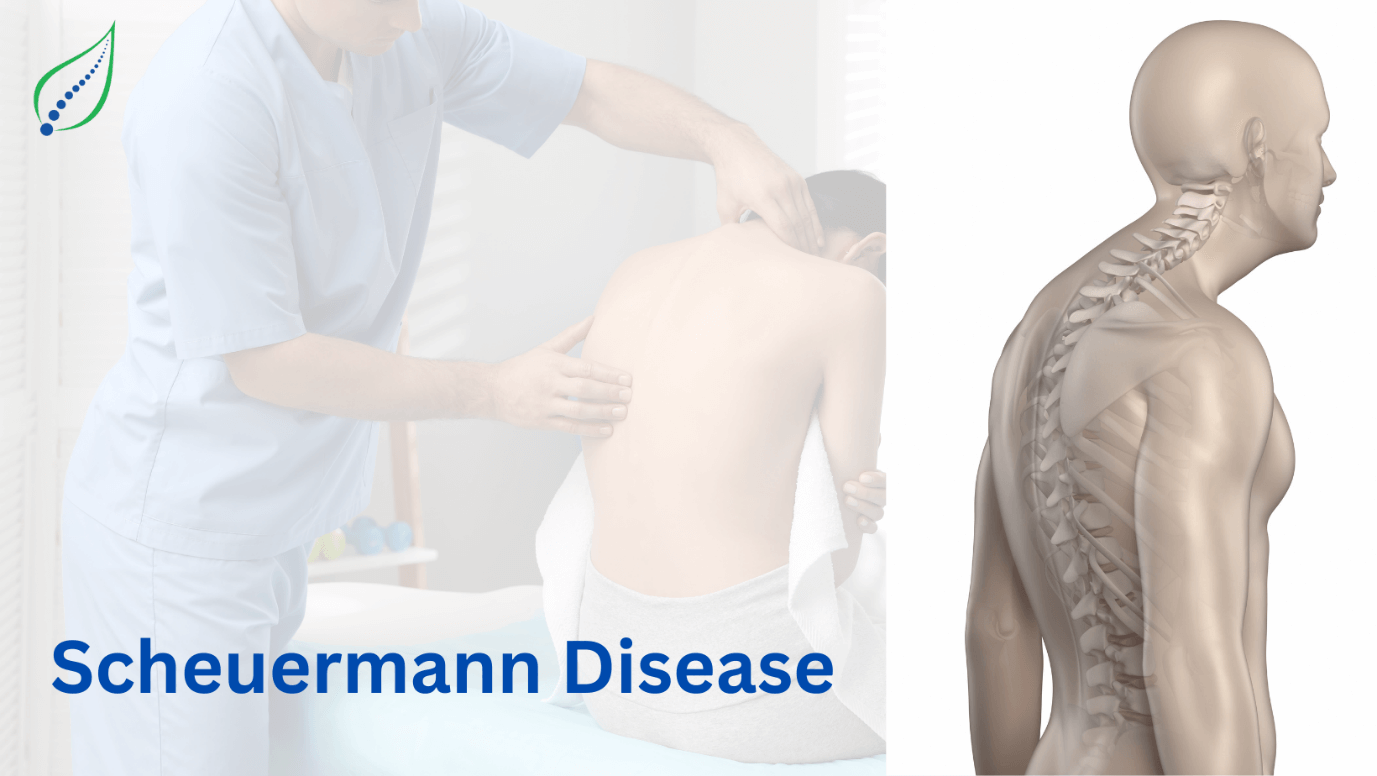
Scheuermann Disease
Scheuermann disease also known as Scheuermann kyphosis or juvenile kyphosis or juvenile discogenic disease which is result of hyper kyphosis in the vertebral bodies. It is a self-limiting skeletal disorder. The kyphosis of thoracic body may be up to 45-75 degrees.
Shoulder Pain
Acromioclavicular Arthropathy
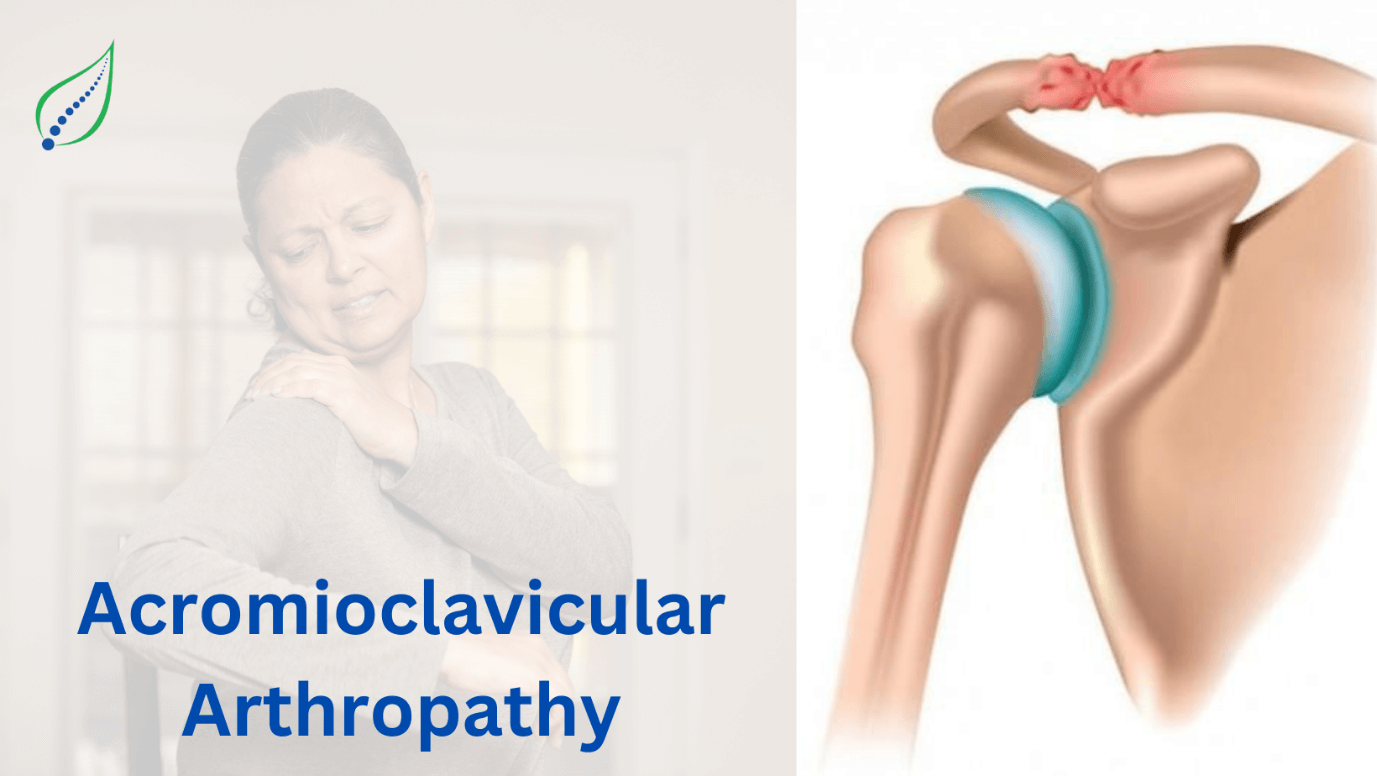
Acromioclavicular Arthropathy
Acromioclavicular arthropathy or acromioclavicular osteoarthritis happens when degenerative changes occur in between clavicle and acromion process resulting in formation of bone spurs and inflammation causing immense pain and restrictive movement of shoulder.
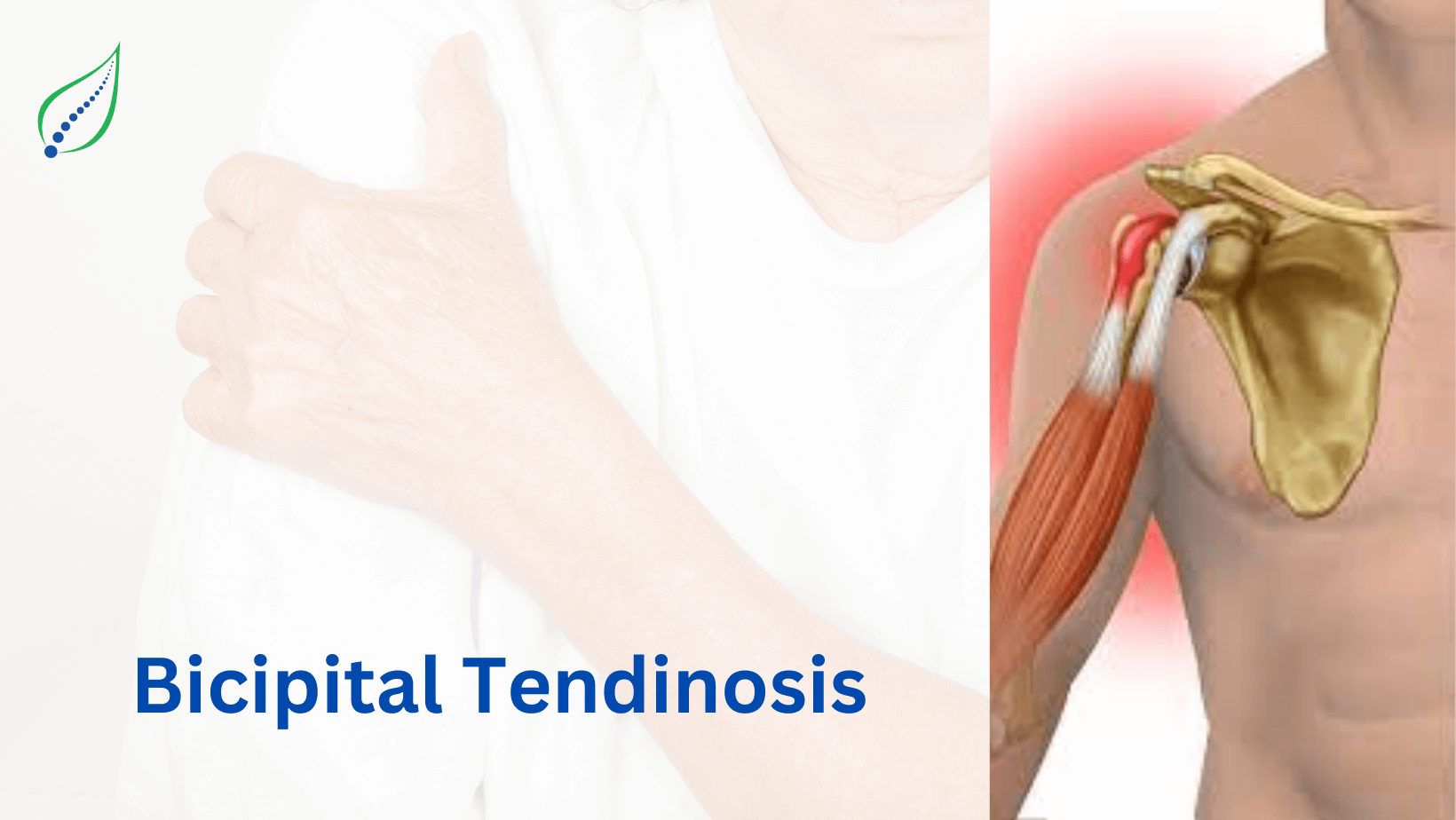
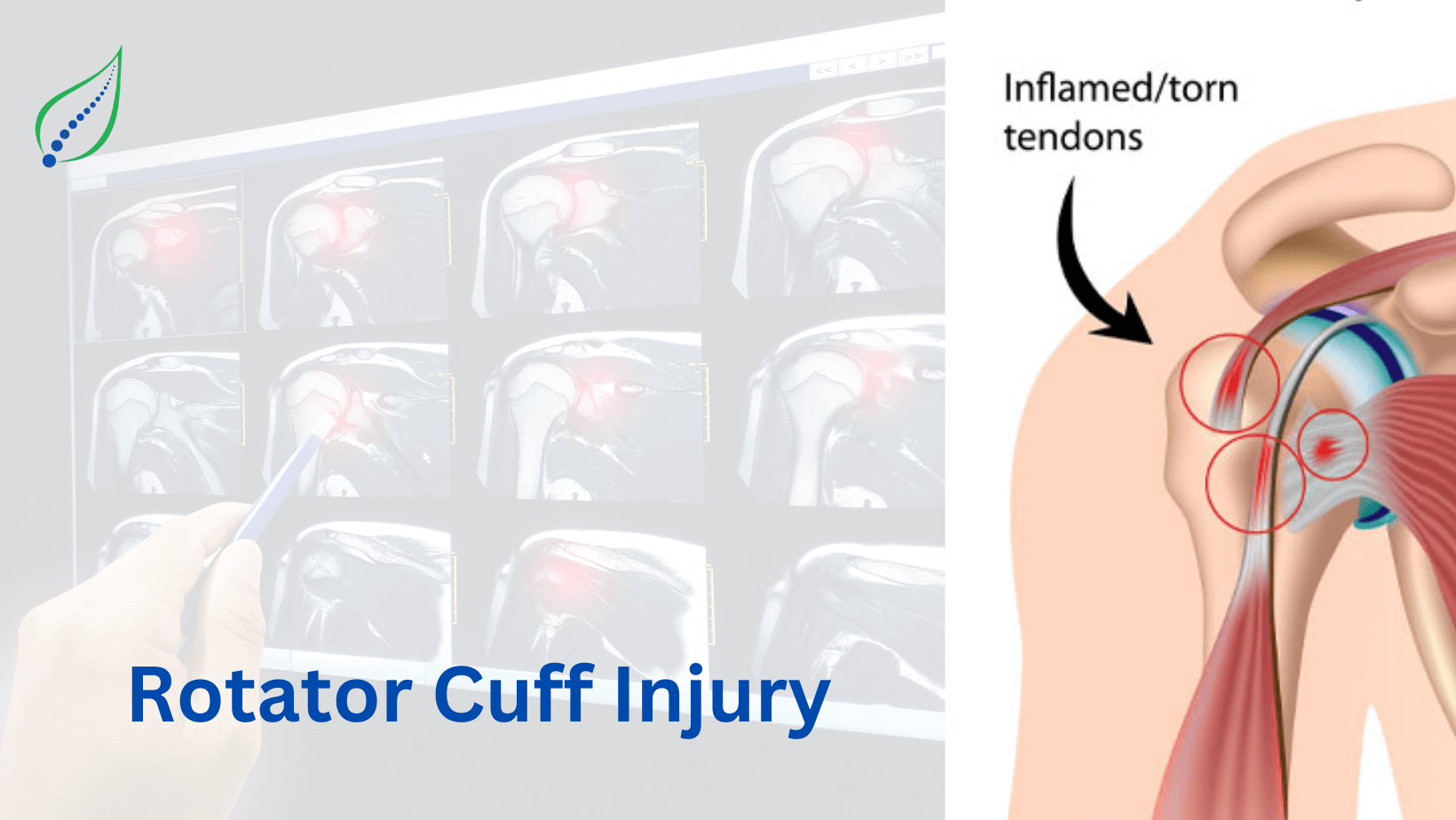
Supraspinatus Tendinosis
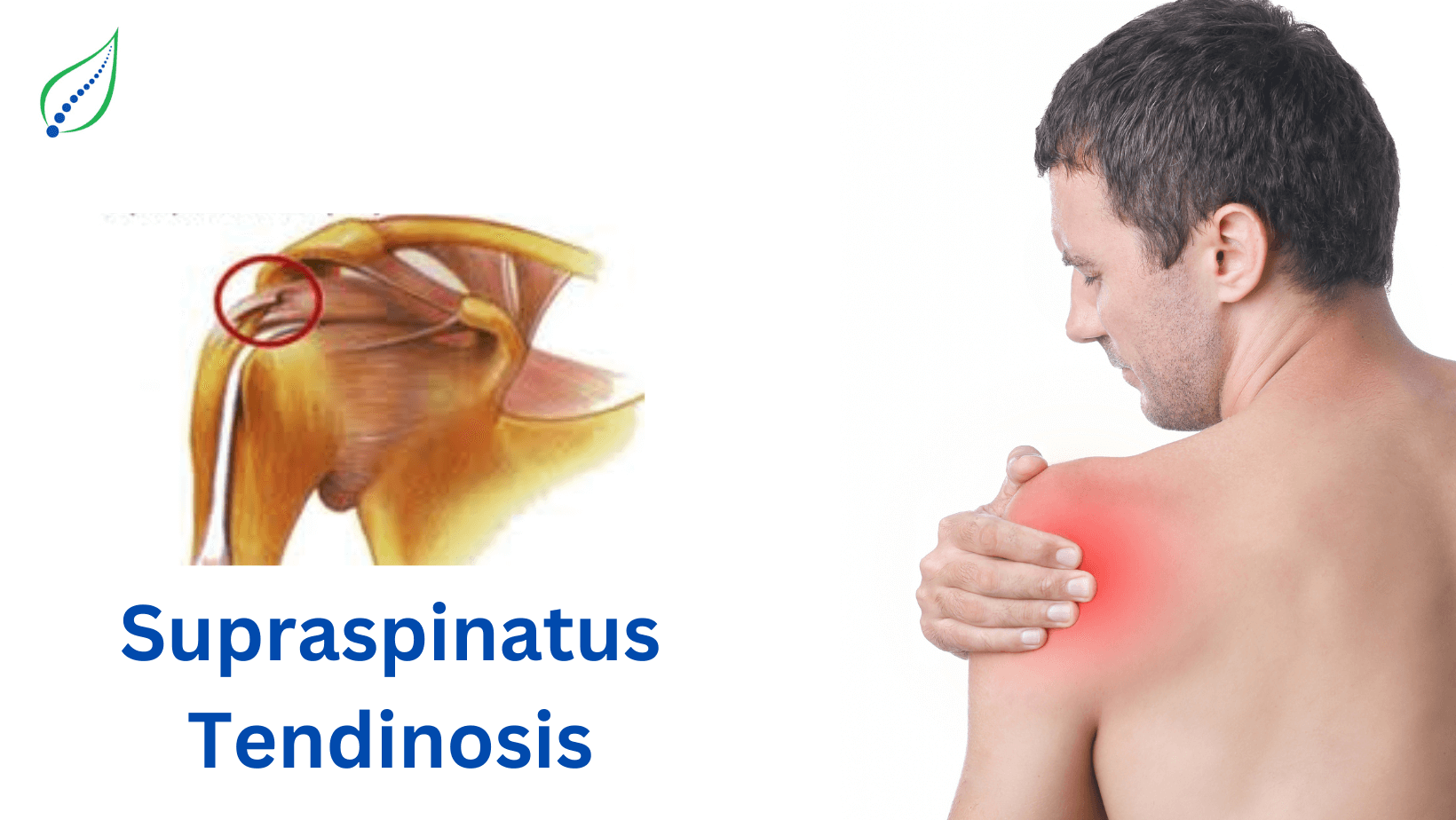
Supraspinatus Tendinosis
One of the leading causes of shoulder pain in middle and old age is Supraspinatus tendinosis. The pain in the shoulder area is usually caused due to repetitive activities leading to a degeneration of the Supraspinatus tendon, which is a part of the rotator cuff.
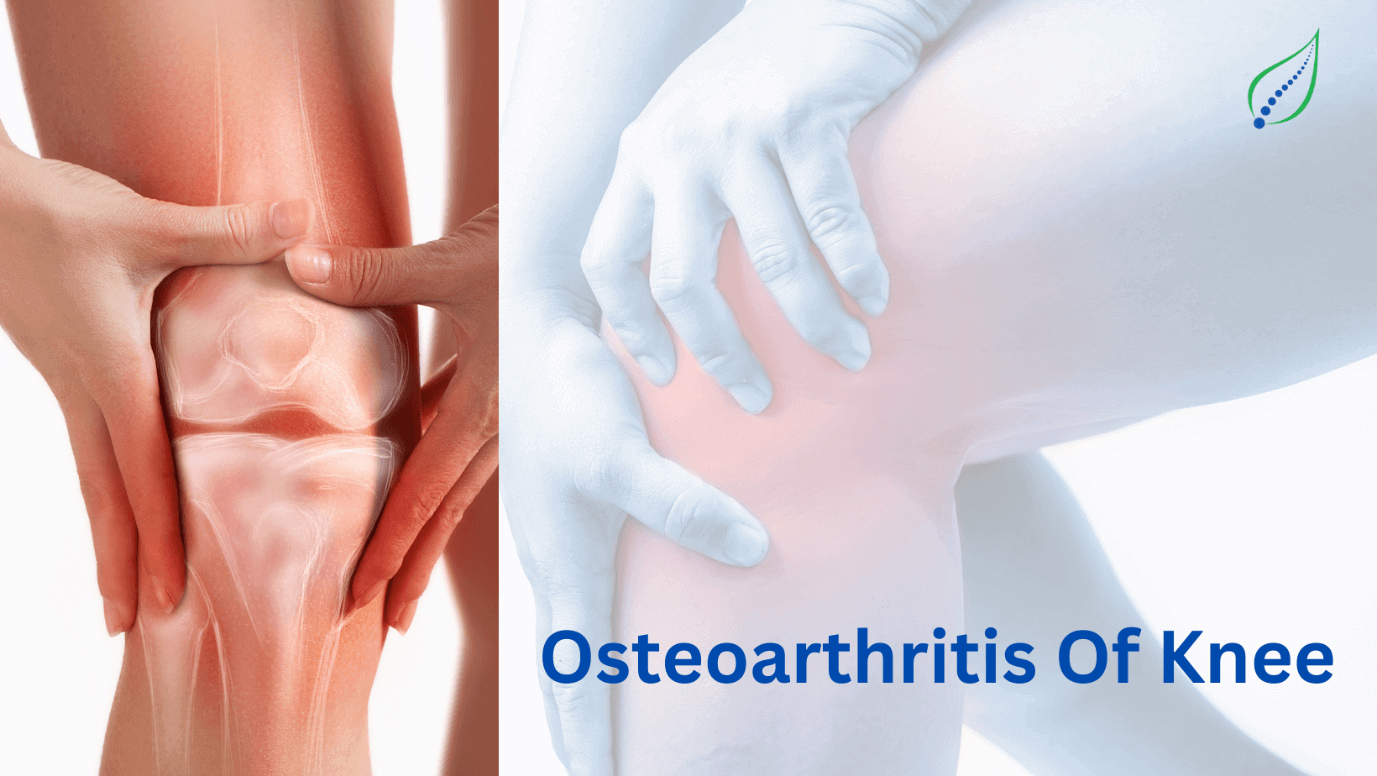
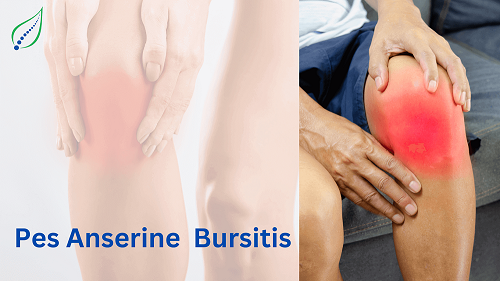
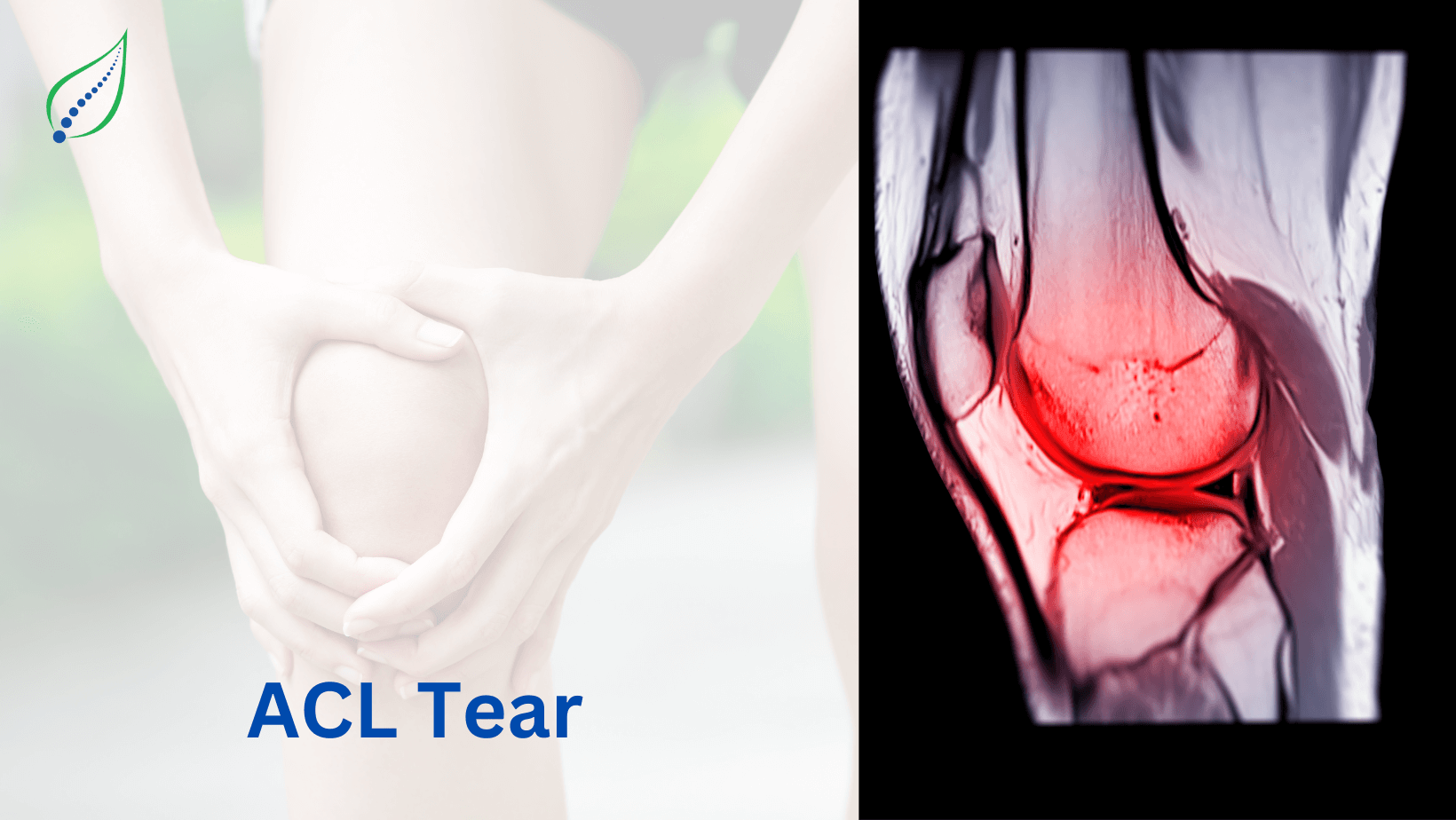
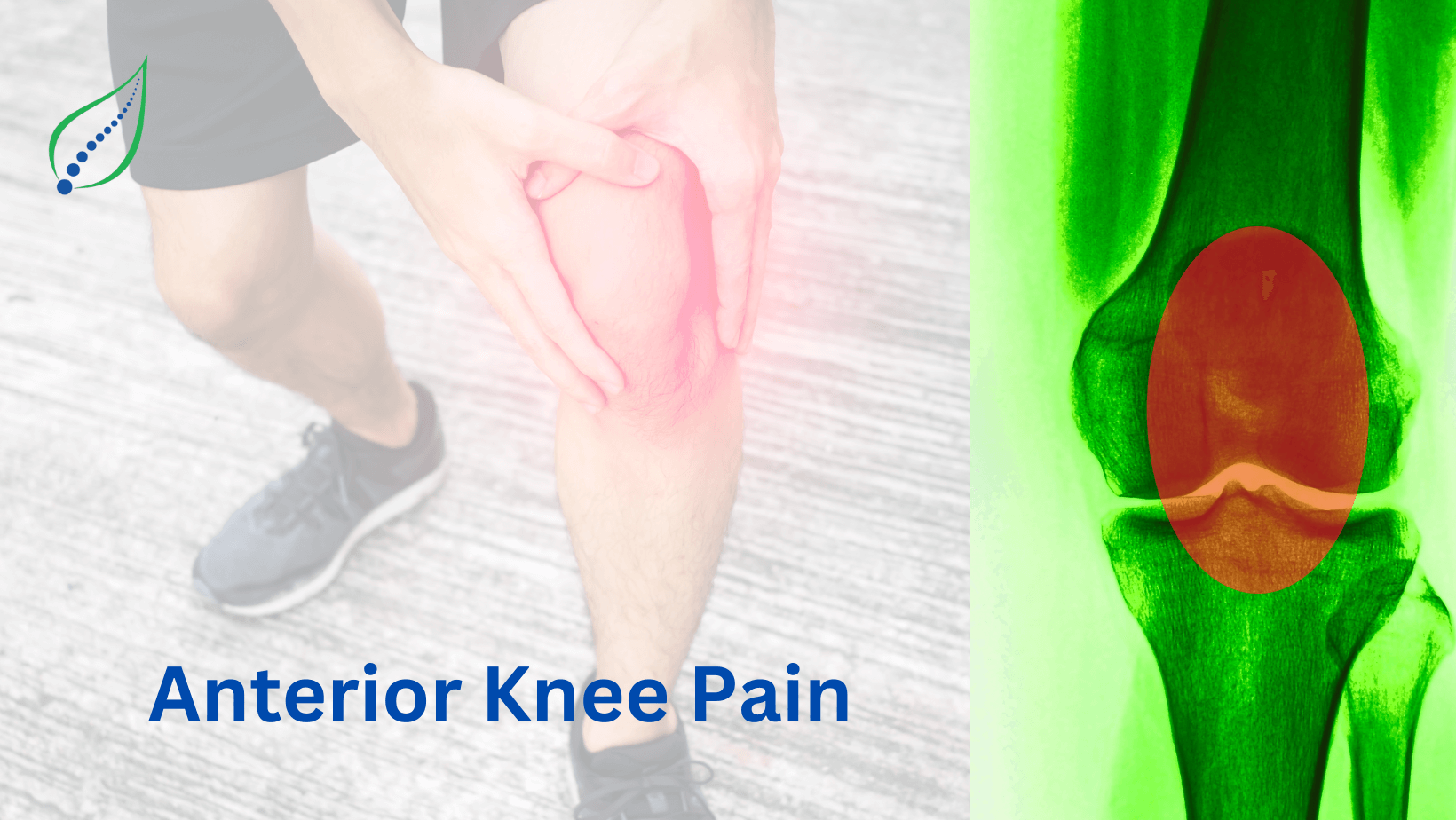
Knee Pain
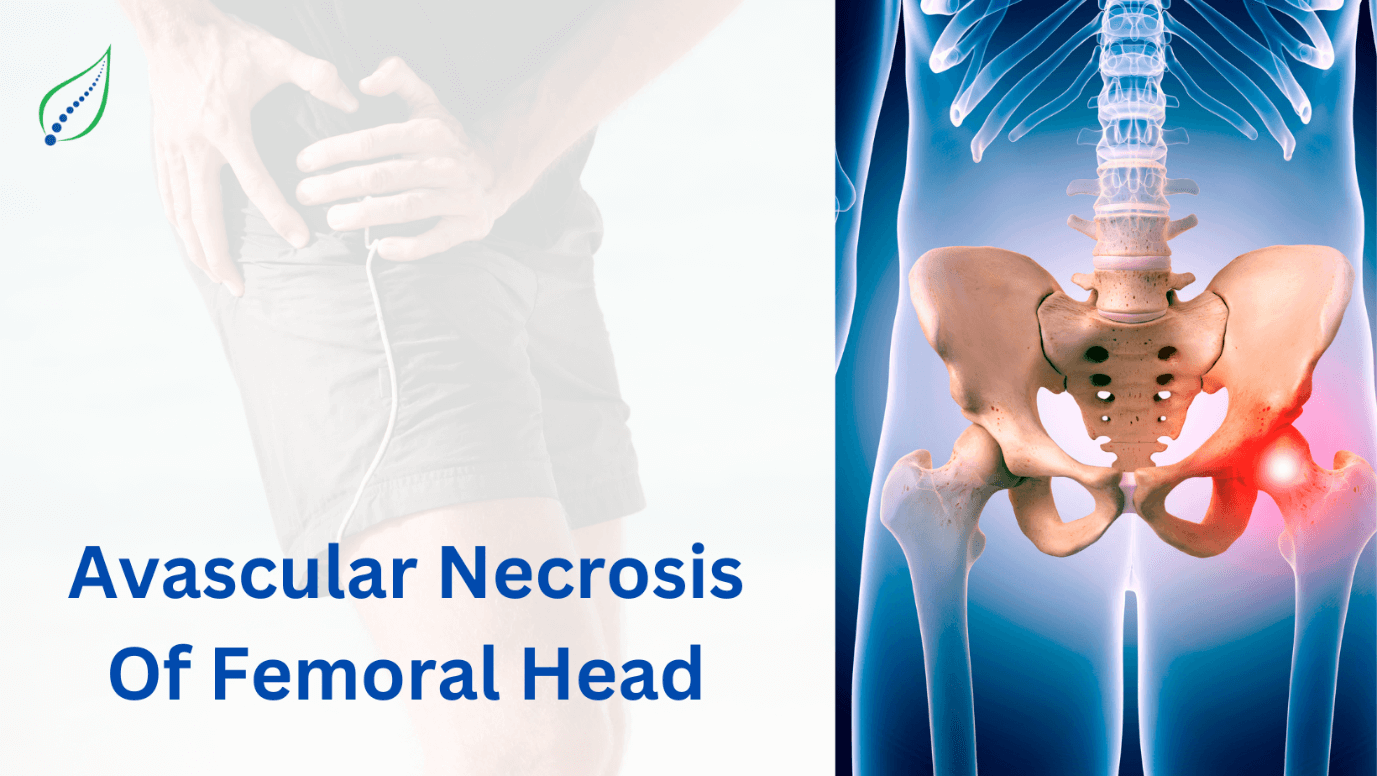
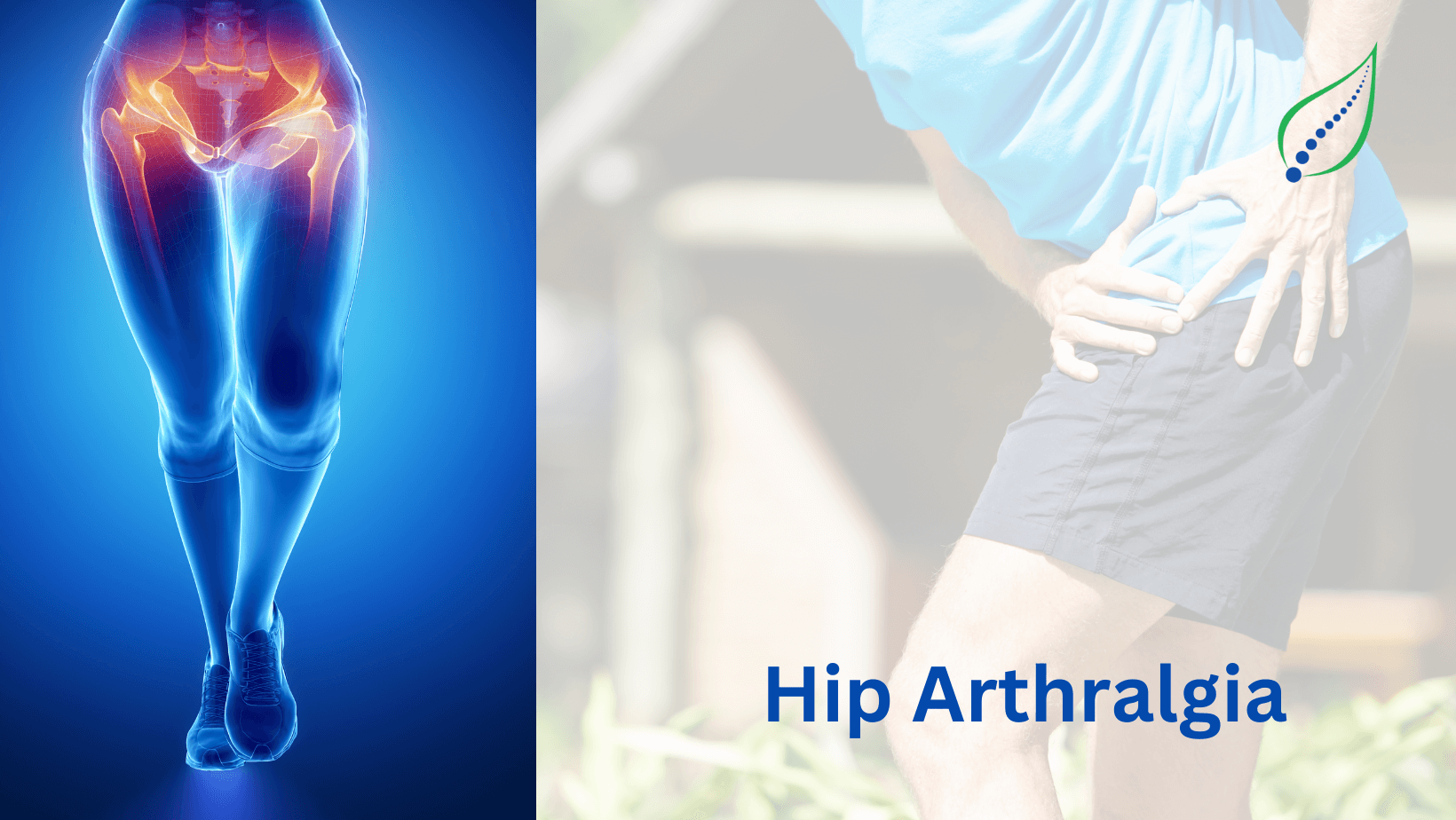
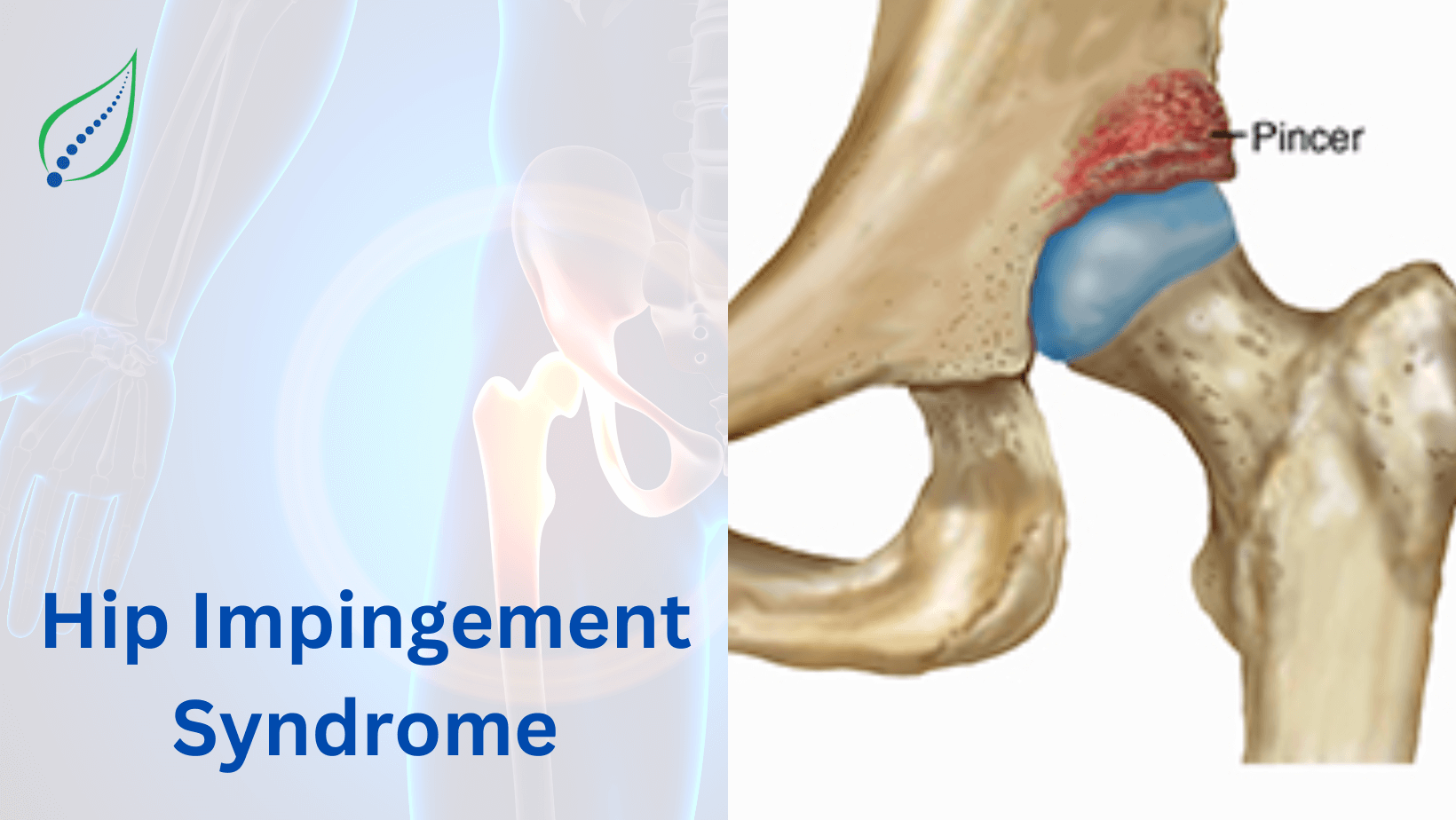
Hip Pain
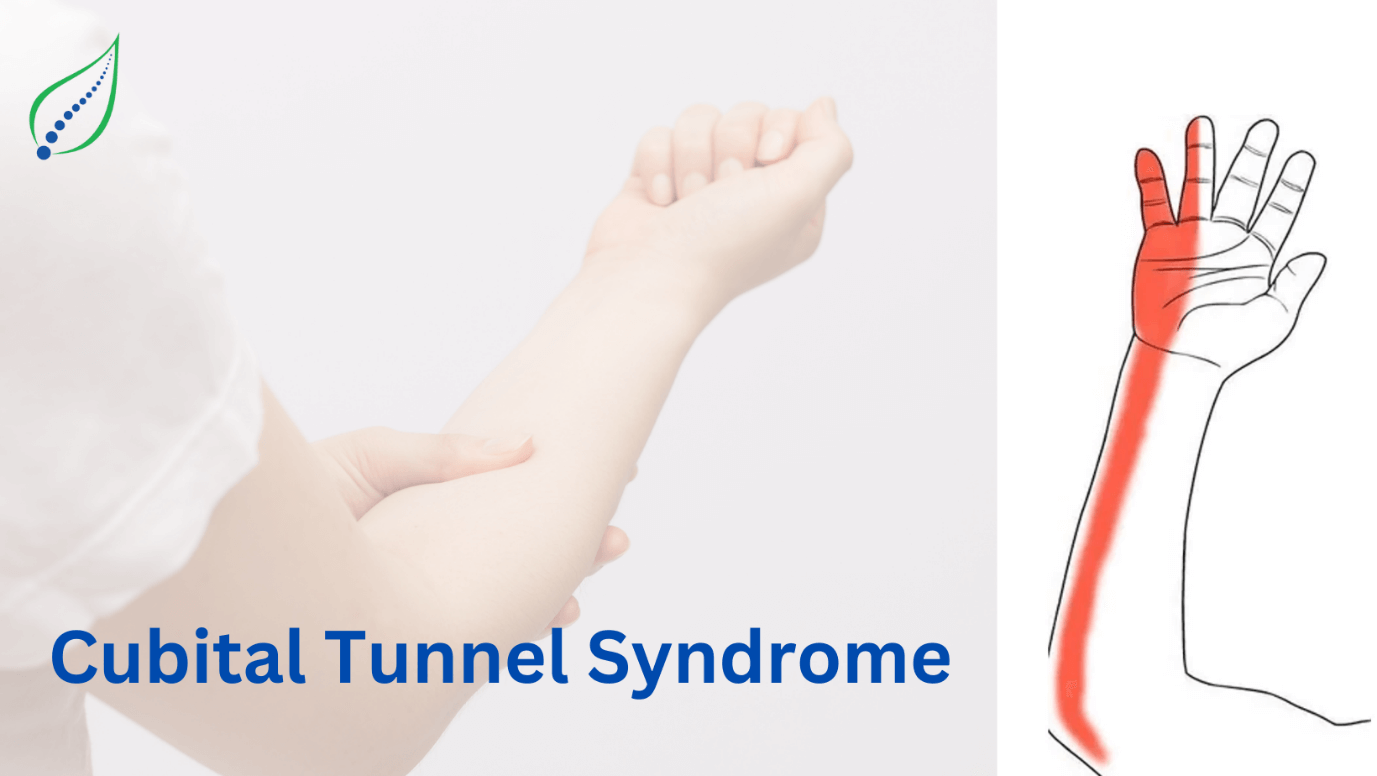
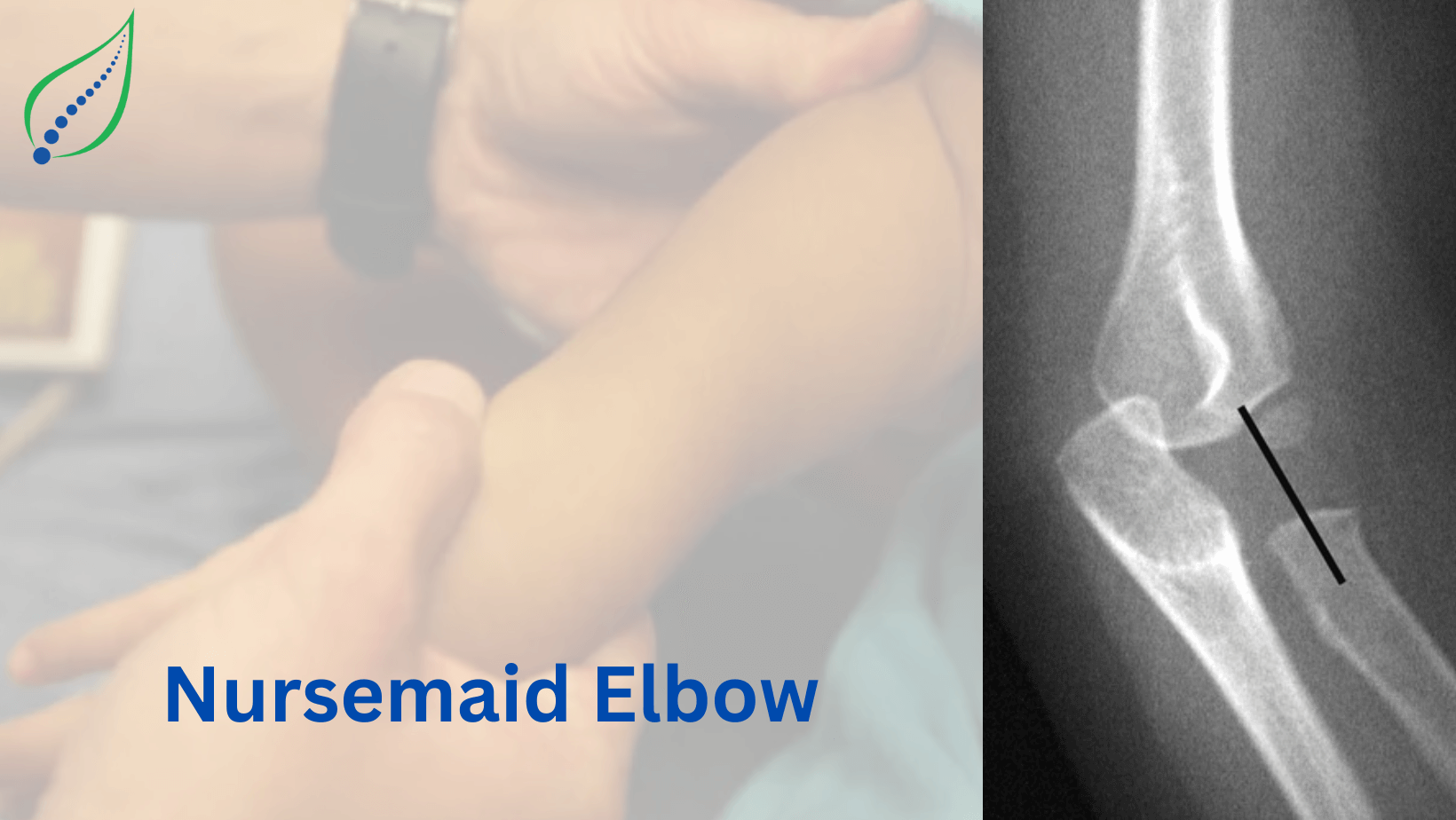
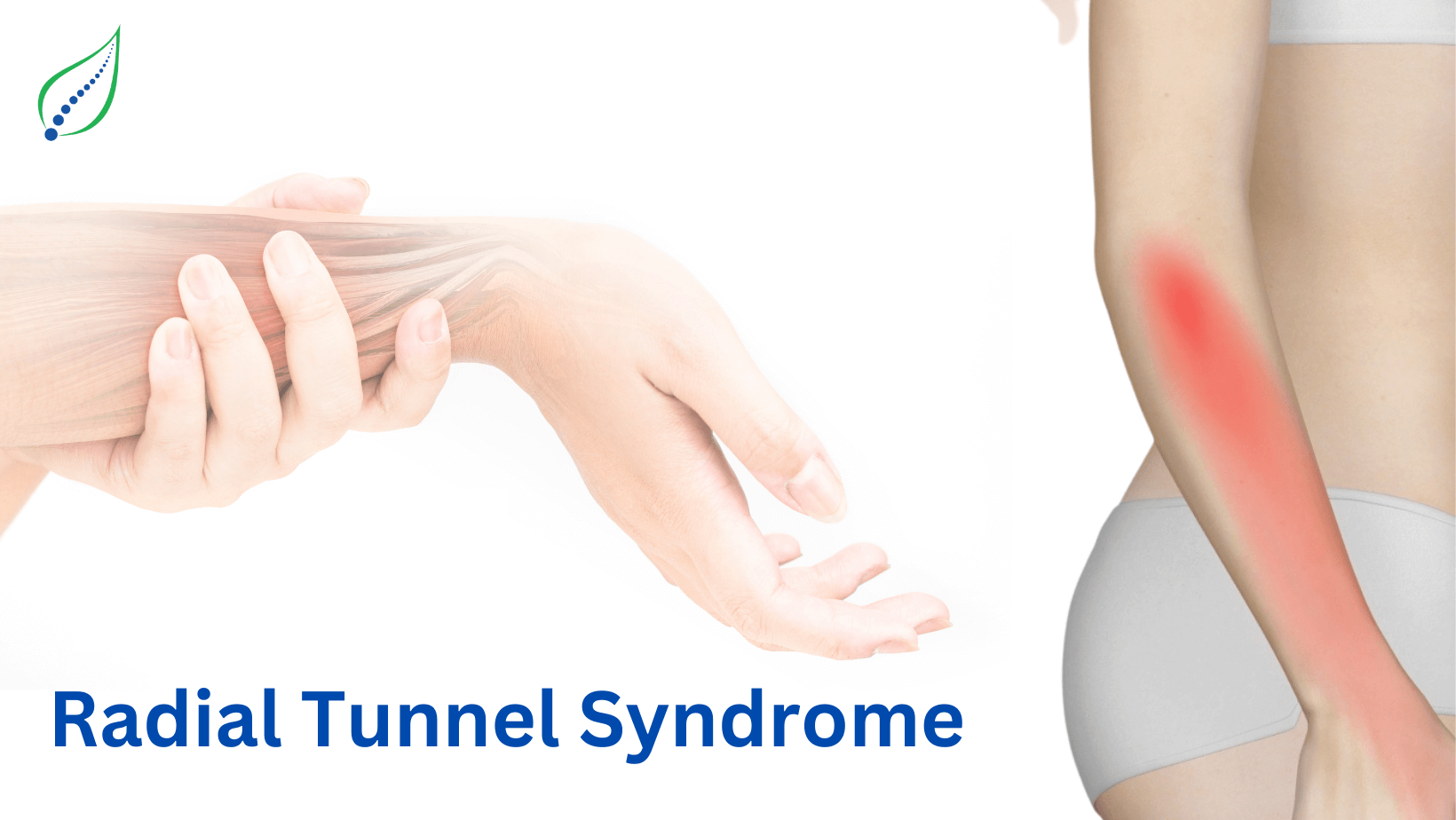
Elbow Pain
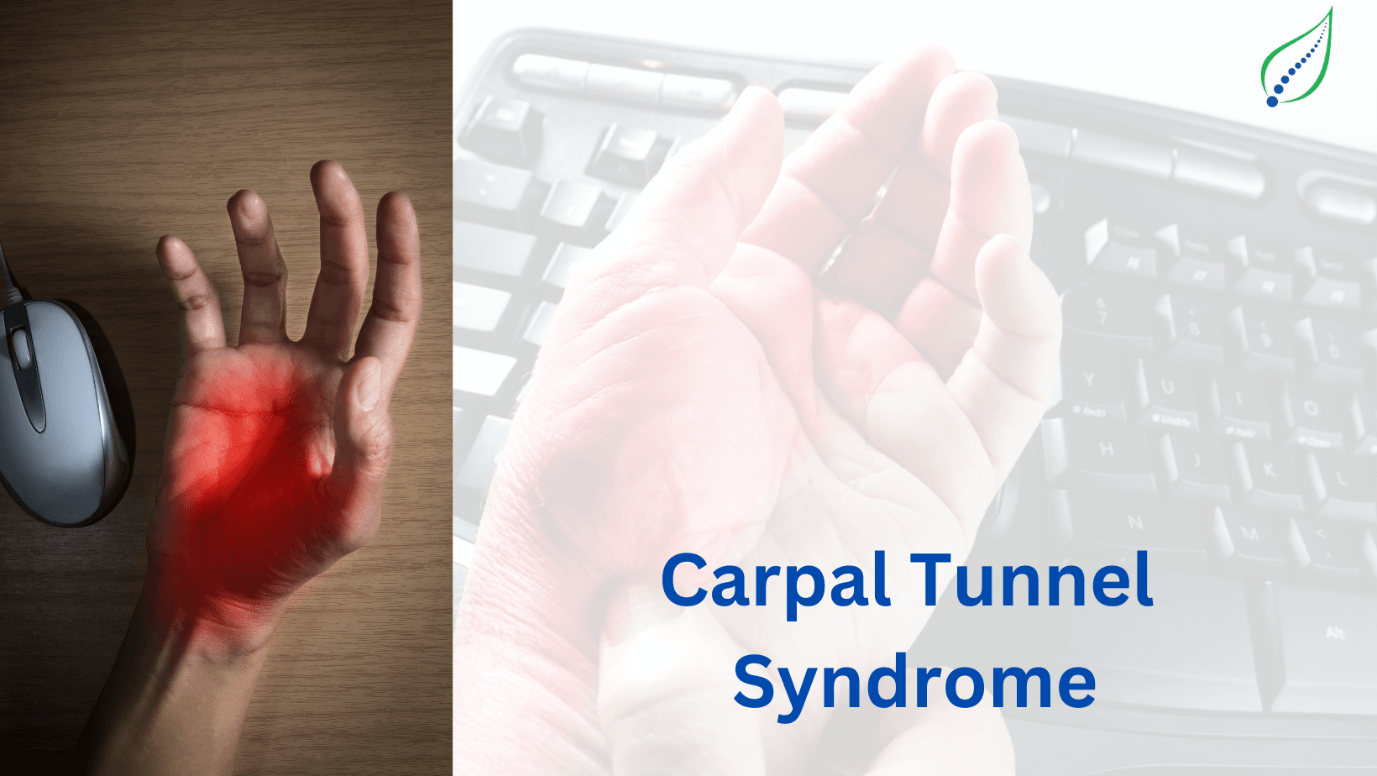
Hand & Wrist Pain
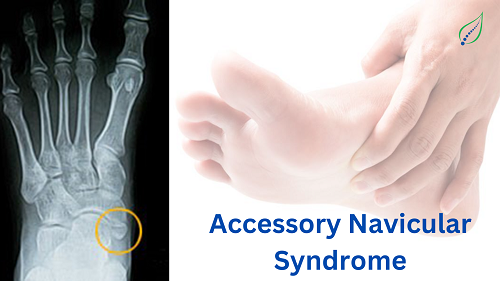
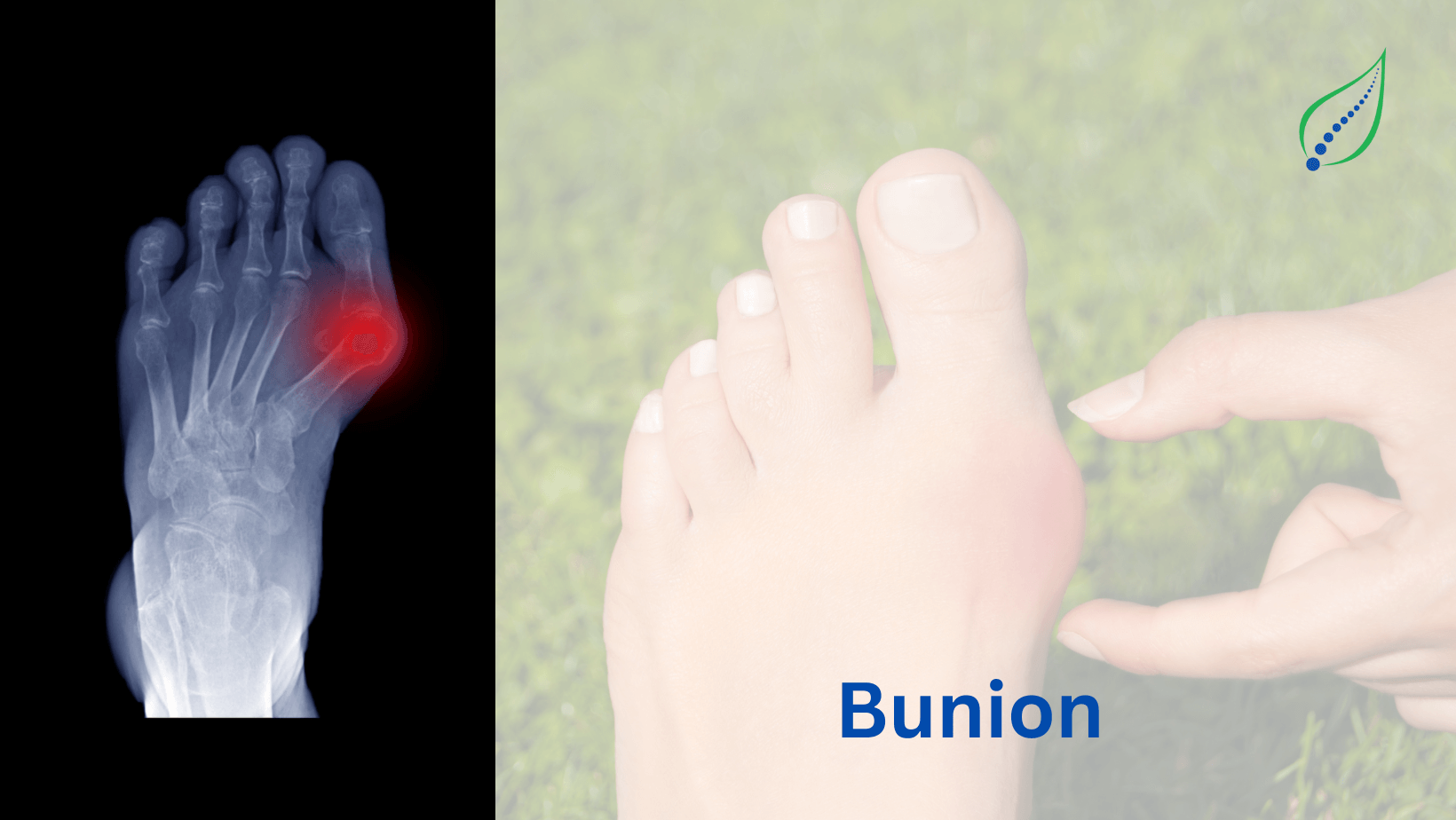
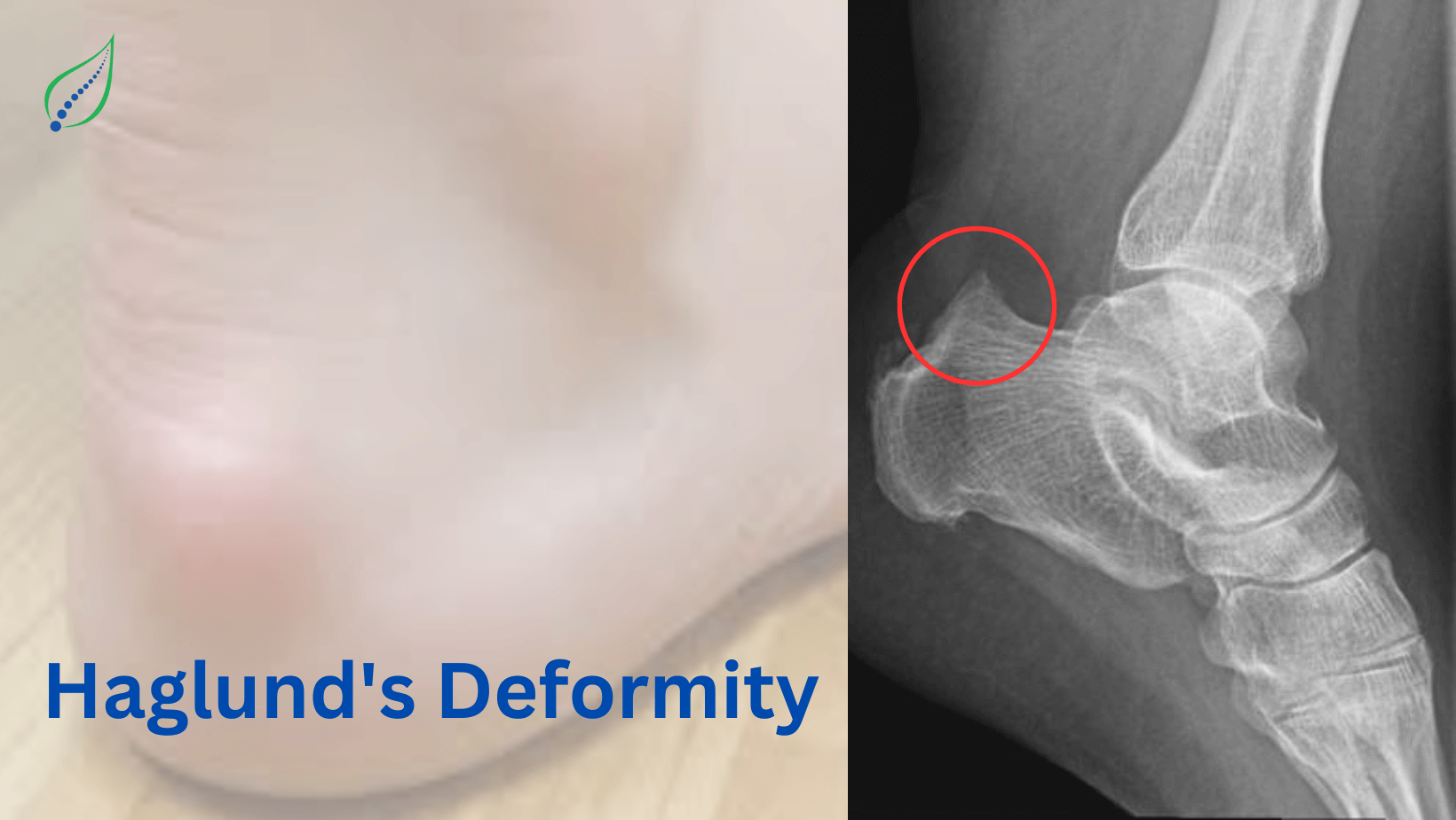
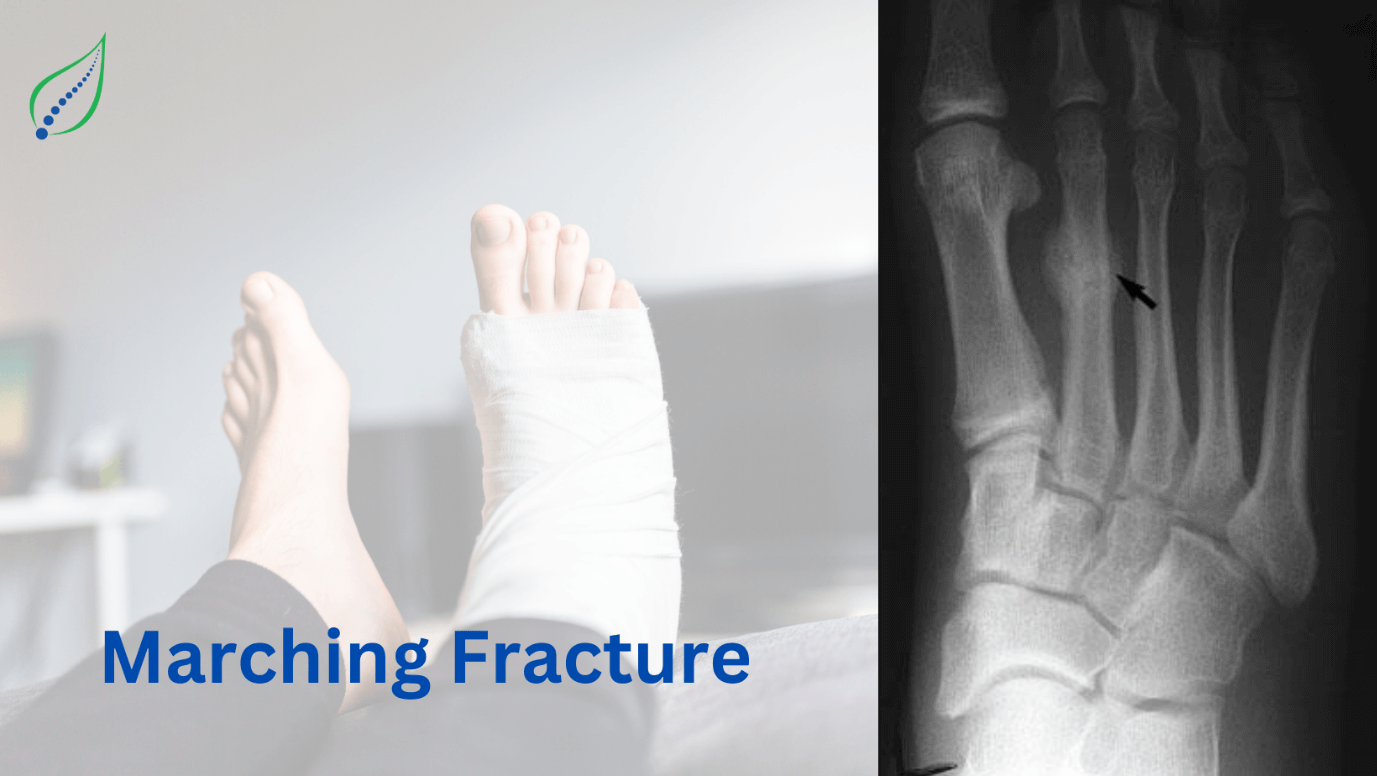
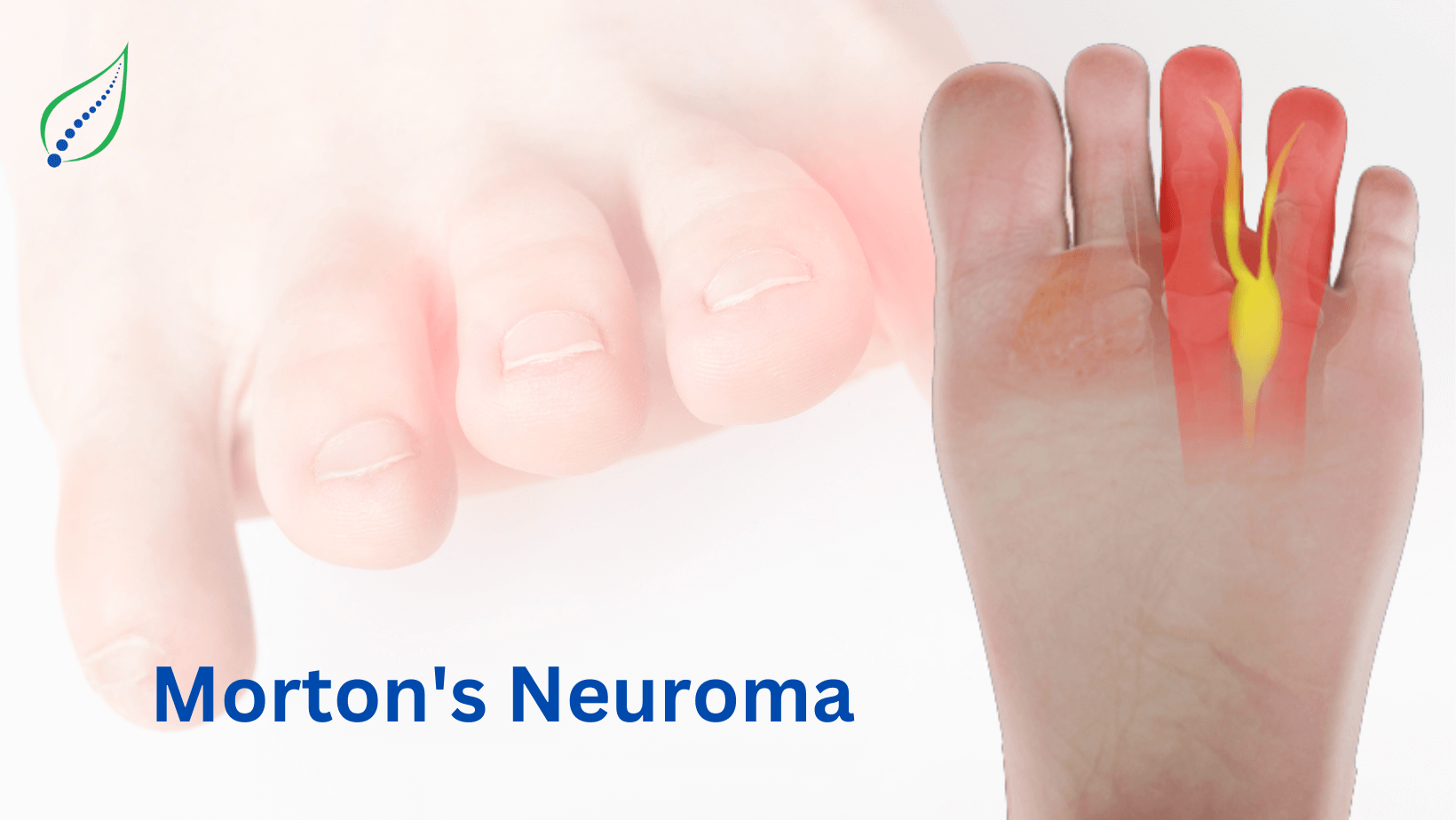
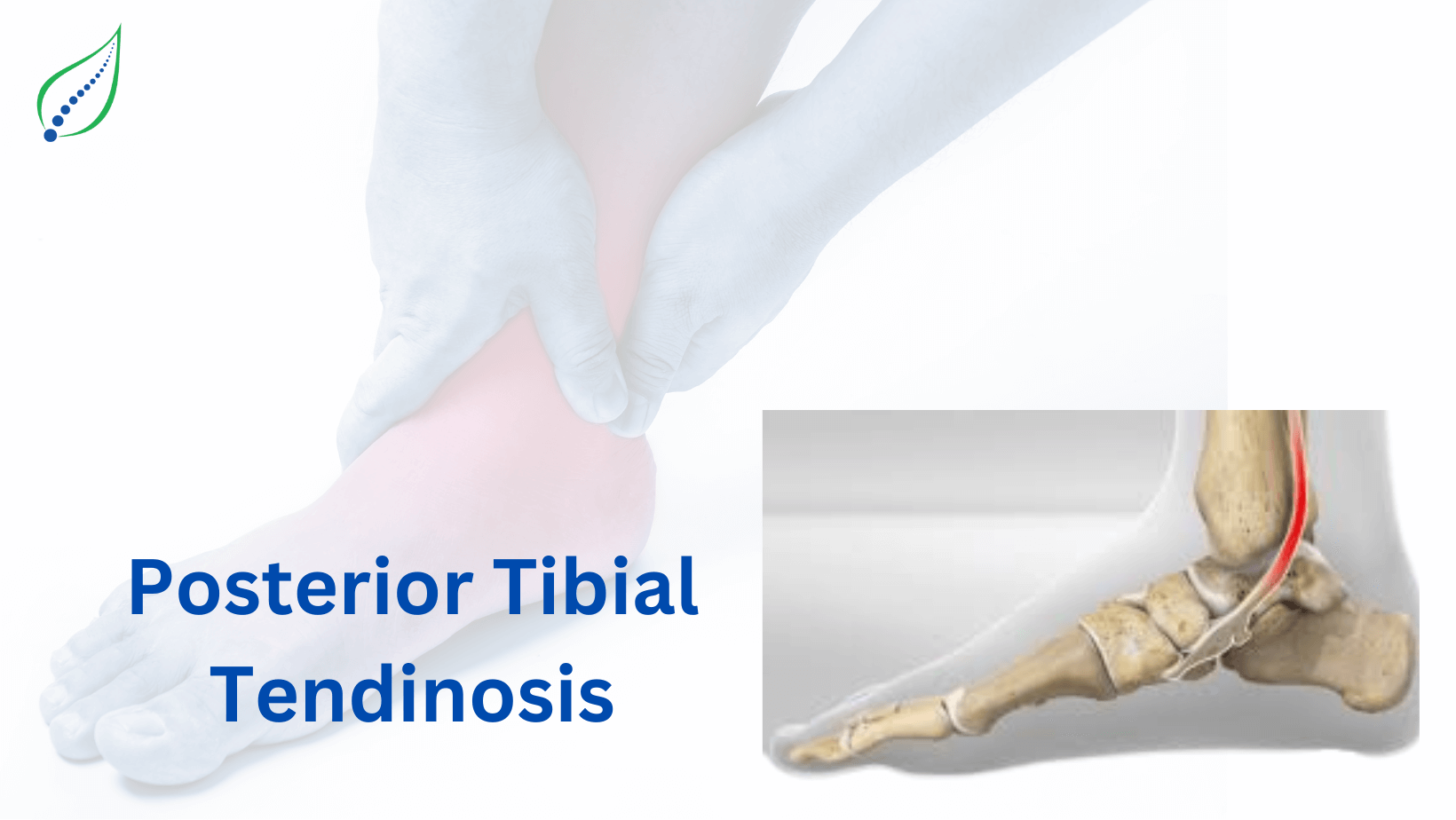
Ankle and Foot Pain
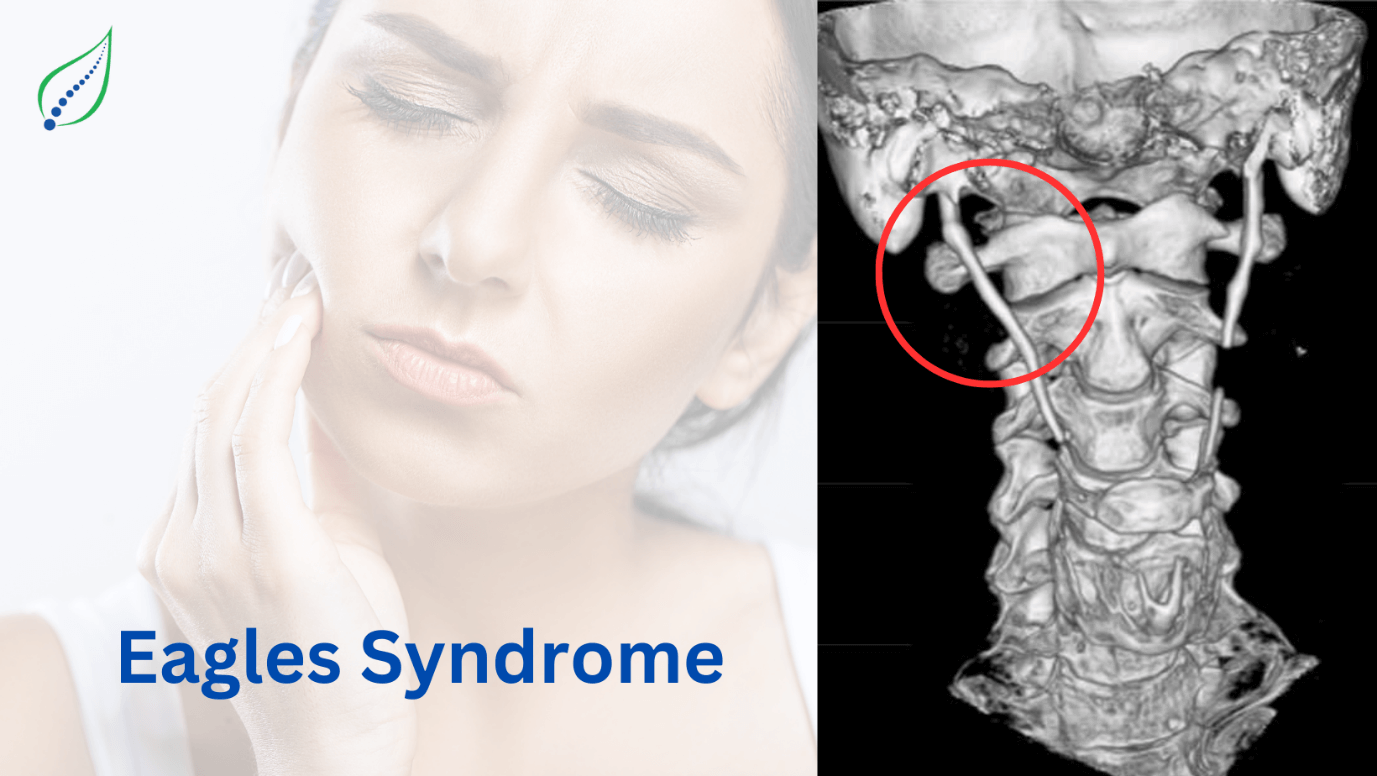
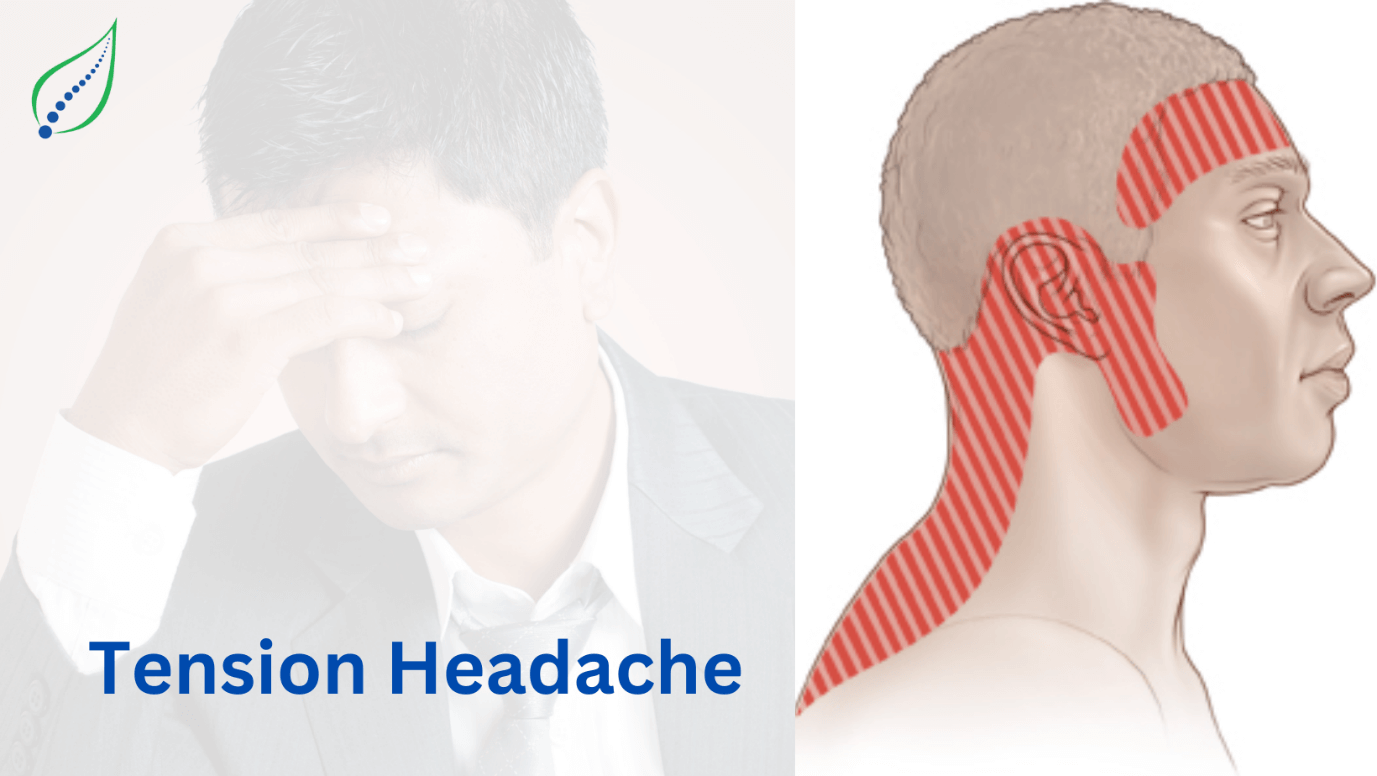
Headache
Leg Pain

Iliotibial Band Syndrome
Iliotibial Band Syndrome
Iliotibial band syndrome is caused by running, hiking, cycling, and activities that require bending the knee in general. The pain is experienced in the outer part of the knee and is a result of the injury of the IT Band, a connective tissue that runs from the outside of the hips, thighs, and crossing the knee joints.
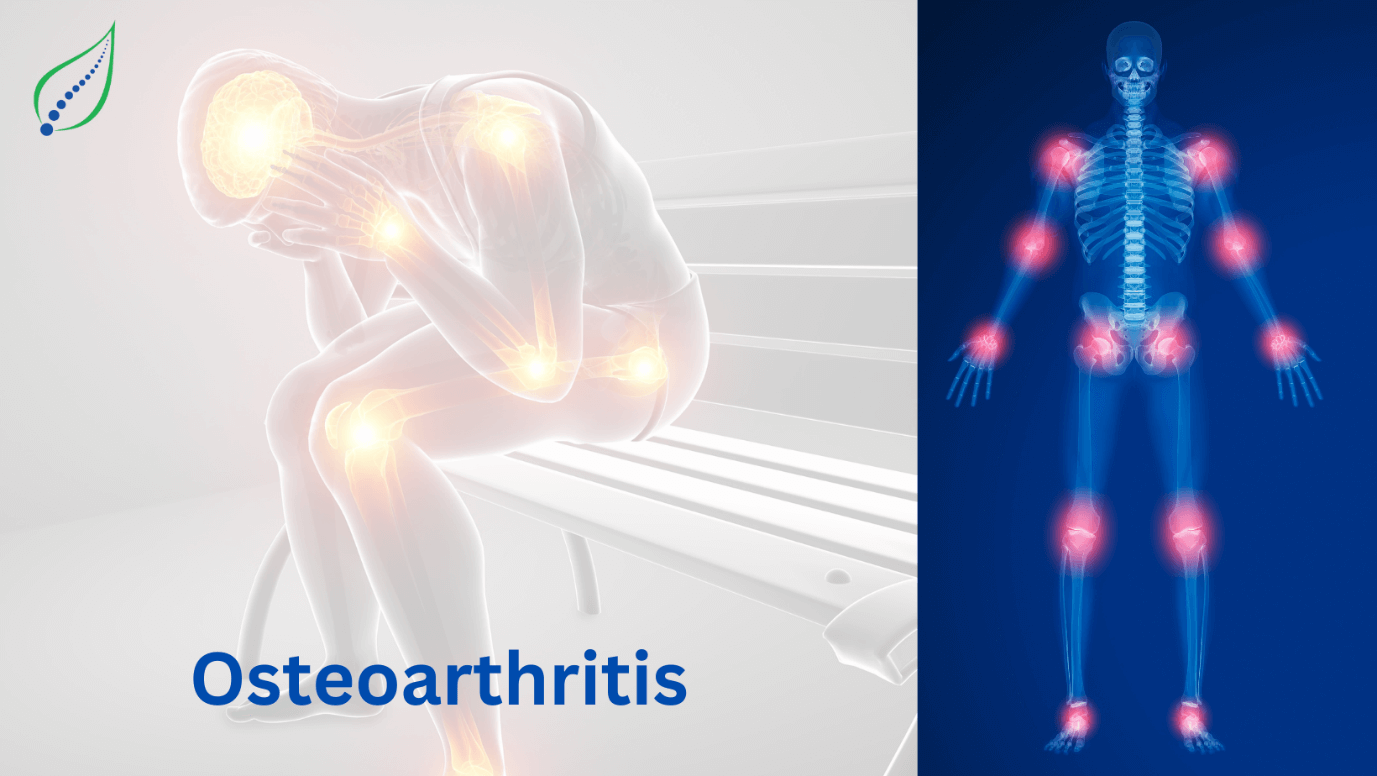
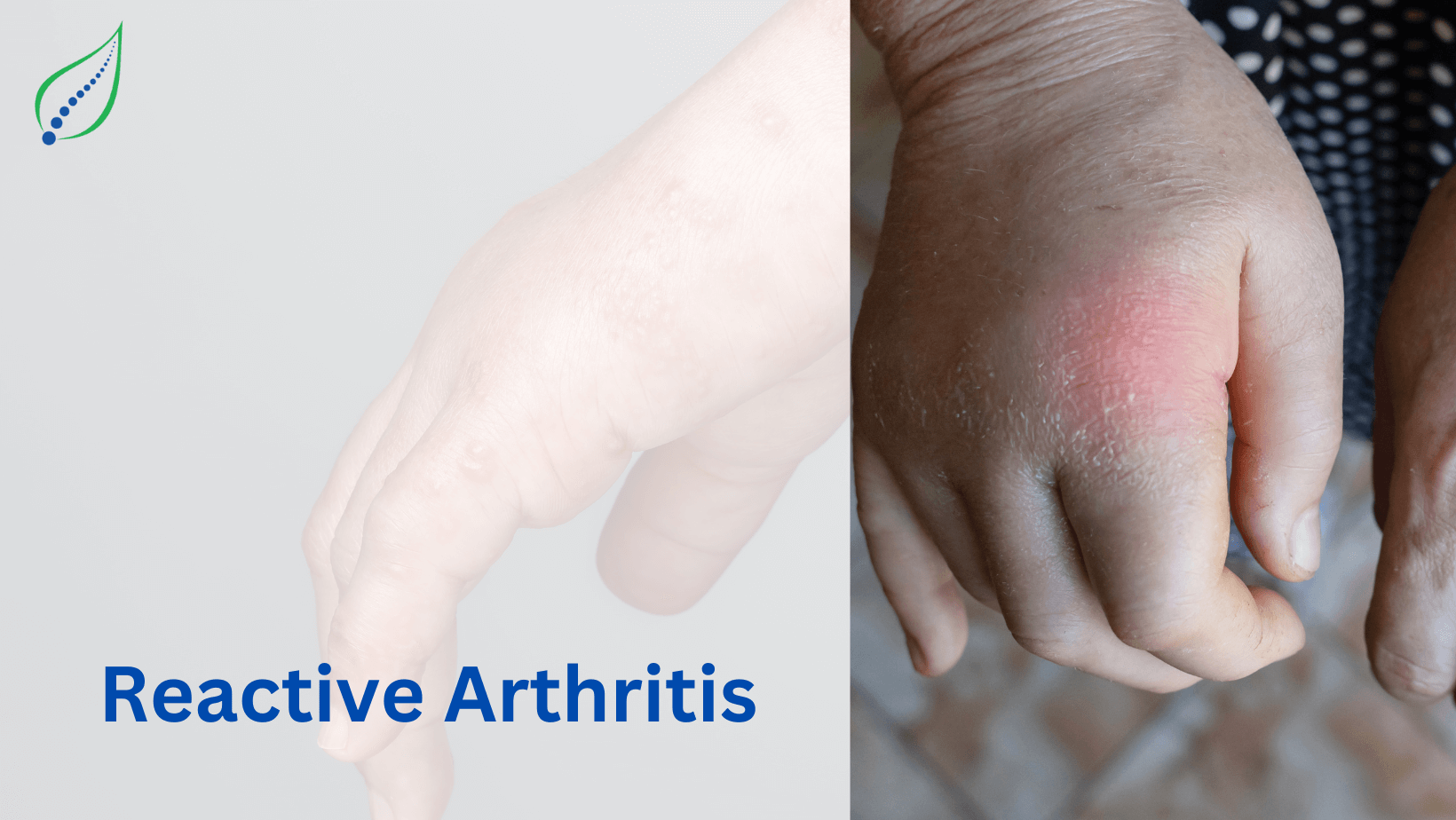
Arthritis
Seronegative Spondyloarthropathy
Seronegative Spondyloarthropathy
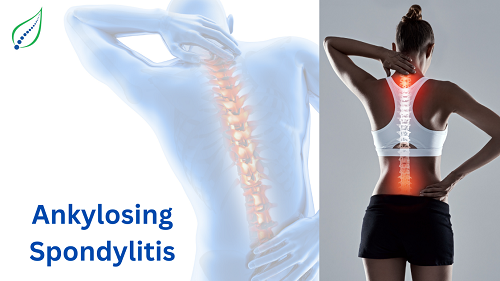
Seronegative spondylarthritis/spondyloarthropathy is a category of inflammatory diseases such as ankylosing spondylitis, psoriatic arthritis, inflammatory bowel disease-associated inflammatory arthritis, and reactive arthritis. It affects areas where ligaments and tendons attach to bones called “entheses”.
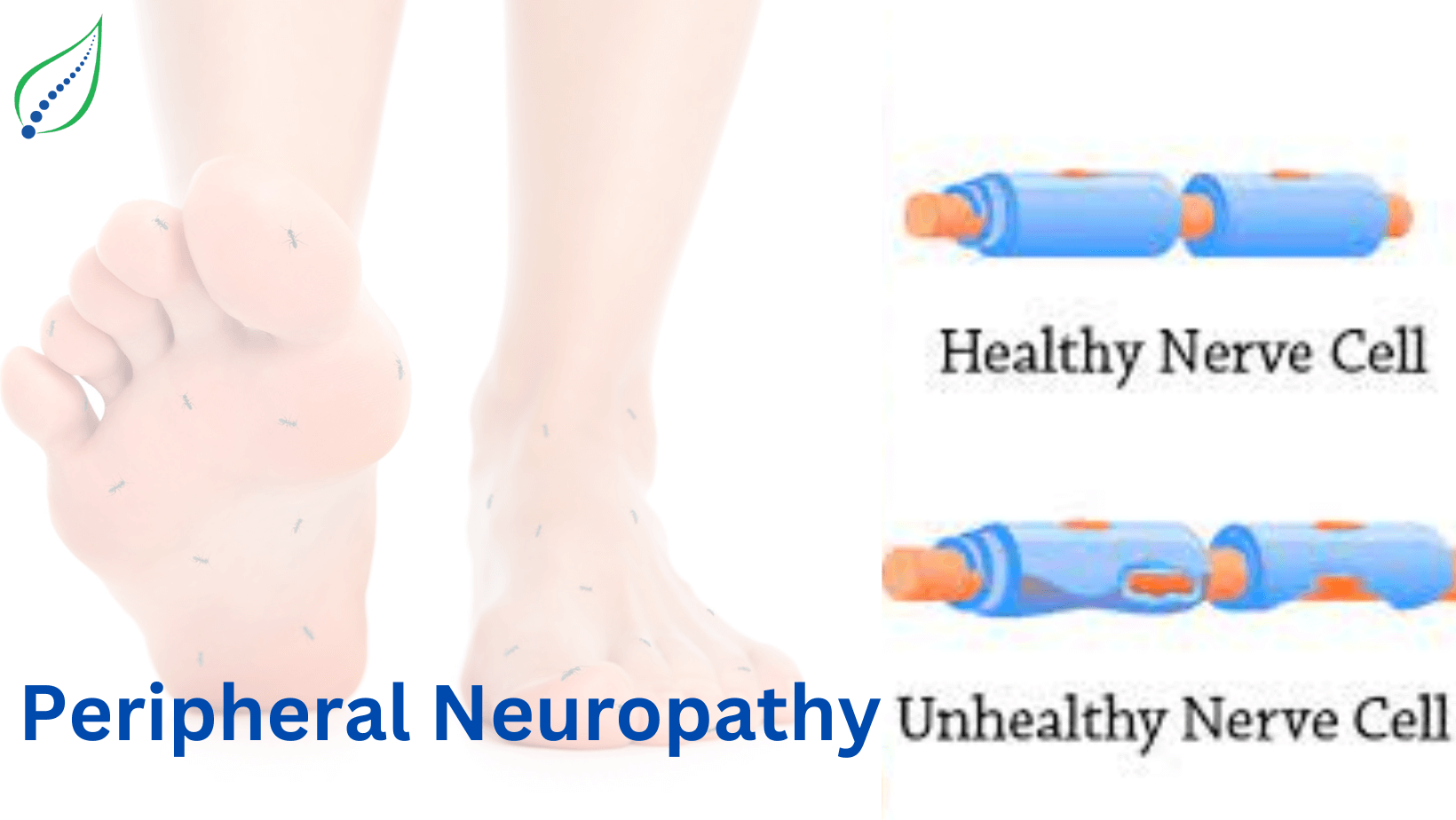
Neuropathy
Alcoholic Neuropathy
Alcoholic Neuropathy
Drinking too much can alter level of nutrients such as thiamine, folate, Vitamin B6 and Vitamin B12 which are important for nerve conduction. Deficiency of these vitamins due to chronic alcoholism results in alcoholic neuropathy. It affects the movement and sensation of arms and legs.
Other
MSK Tumours
MSK Tumours
MSK Tumours (Musculoskeletal Tumours) are the abnormal growth of cells within the bone, muscles, cartilages which can be malignant or benign. If they are malignant, they are considered sarcomas e.g., osteosarcoma. A major concern with bone tumours is the development of pathologic fractures.